Sleep disorders can affect our lives in a variety of ways, impacting our mental and physical health. Two sleep disorders that can create confusion are parasomnia and insomnia. While both of them can trigger insomnia-related problems, however, they are distinct in their causes symptoms, and effects on our daily lives.
We will look at the different aspects of insomnia, which is characterized by problems getting to sleep or sleeping, and parasomnia which is characterized by unusual behaviours or experiences while sleeping. Understanding the differences between these two conditions is vital to a correct diagnosis and efficient management, resulting in better quality sleep and overall well-being.
Explanation of Insomnia
A sleep disorder called insomnia is characterized by frequent difficulties in establishing or maintaining sleep despite having the ability for and the need to rest. It is often a result of inadequate or inadequate quality sleep, which results in daytime fatigue, irritability, and impaired cognitive performance. Sleeping disorders can be permanent or chronic issues and can have a variety of causes, like anxiety, stress, or medical issues, as well as lifestyle elements.

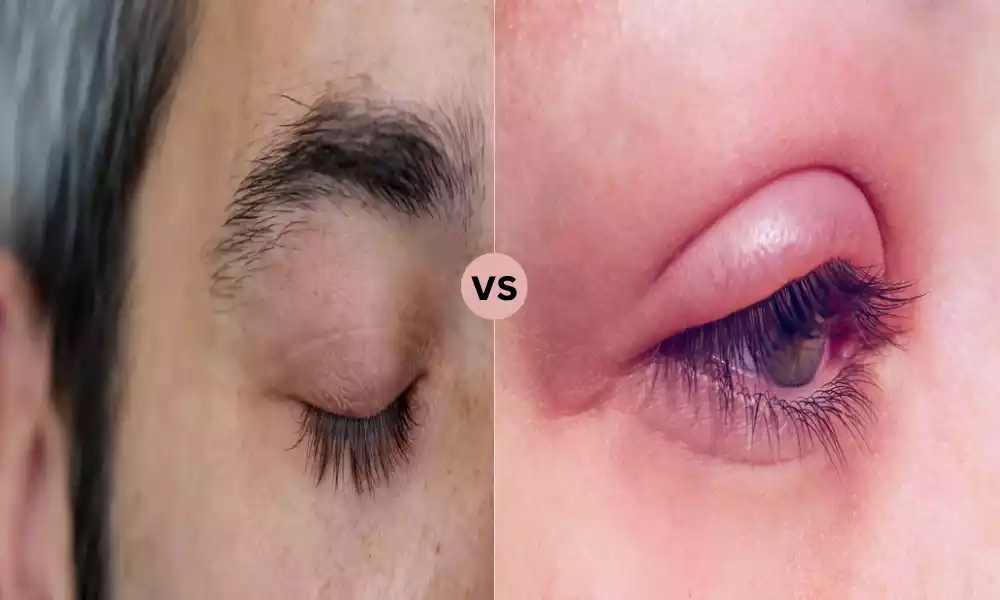
Explanation of Parasomnia
Parasomnia is the term used to describe a variety of sleep disorders that are characterized by abnormal behavior such as movements, experiences, or even sensations that take place in sleep.
These experiences and behaviors tend to be involuntary and vary from basic movements such as sleep talking, to more complicated actions like sleepwalking and night terrors.
Parasomnias can manifest at different phases of sleep, like the non-REM (rapid eye movements) as well as REM sleep. They typically alter regular sleep patterns. The reason for parasomnia could be different, and include the genetics of the issue or stress, sleep deprivation, or any other sleep conditions.

Importance of distinguishing between insomnia and parasomnia
Differentiating between insomnia and parasomnia is essential for a number of reasons:
- Accurate Diagnosis:
- Parasomnia and sleep disorders require different strategies for diagnosis and treatment. The ability to pinpoint the precise sleep disorder allows medical experts to offer targeted treatments.
- Tailored Treatment:
- Insomnia usually involves issues with sleep initiation and maintenance and is treated using cognitive-behavioral treatments, medications or lifestyle modifications. Parasomnia however requires specialized strategies for managing abnormal behaviors when you sleep.
- Safety Concerns:
- Sleepwalking as well as night terrors may present safety risks for individuals as well as those in their vicinity. The distinction between these two disorders aids in the implementation of appropriate safety measures.
- Sleep Quality:
- Sleep quality is affected by insomnia because it causes difficulty falling or being asleep. An accurate diagnosis can ensure that treatment plans concentrate on improving the quality of sleep and quality. However, parasomnia can cause disruption to sleep patterns through unexpected awakenings or awakens.
- Psychological Impact:
- Sleepiness is linked to depression, fatigue during the day, and cognitive impairment. In the event of addressing insomnia, it can result in better mental well-being. In addition, insomnia can impact the mental health of a person due to its disruptive nature as well as the possibility of experiencing distressing feelings in sleep.
- Long-Term Health:
- Both sleep and insomnia can be long-lasting health risks in the event that they are not treated. Chronic insomnia is associated with a higher risk of a variety of diseases, including depression and cardiovascular disease. A proper diagnosis and treatment can lower the risk.
- Avoiding Mismanagement:
- Incorrectly diagnosing one sleep disorder for another can result in unproductive or even harmful treatments. For example, the treatment of insomnia using medications could cause more parasomnias.
- Quality of Life:
- Achieving a healthy balance between sleep and other problems, be it sleepiness or parasomnia, could greatly improve a person’s well-being by enhancing sleeping patterns, reducing impairments in the daytime, and reducing psychological distress.
Separating parasomnia and insomnia is vital to ensure patients receive the correct diagnosis as well as treatment and support required to address their particular sleep-related problems, which ultimately leads to improved quality sleep and safety as well as general health.
Comparison Table of Insomnia and Parasomnia
Here’s a comparison table highlighting the key differences between insomnia and parasomnia:
| Aspect | Insomnia | Parasomnia |
|---|---|---|
| Definition | Difficulty falling asleep or staying asleep | Abnormal behaviors or experiences during sleep |
| Timing of Symptoms | Typically during the process of falling asleep, staying asleep, or early morning awakening | During various stages of sleep, including non-REM and REM sleep |
| Common Symptoms | – Difficulty falling asleep – Frequent awakenings during the night – Early morning awakenings – Daytime fatigue and sleepiness | – Sleepwalking (somnambulism) – Night terrors (sleep terrors) – Sleep talking (somniloquy) – Sleep-related eating disorder (SRED) – REM behavior disorder (RBD) – Sleep paralysis |
| Causes | – Stress – Anxiety – Medical conditions – Medications – Lifestyle factors | – Genetics – Stress – Sleep deprivation – Other sleep disorders |
| Impact on Daily Life | – Fatigue and daytime sleepiness – Impaired cognitive function – Mood disturbances – Reduced quality of life | – Safety concerns (e.g., risk of injury during sleepwalking) – Sleep disruption for self and bed partner – Potential for psychological distress |
| Diagnosis | – Clinical assessment – Sleep diaries – Sleep studies (polysomnography) | – Clinical assessment – Observation by a bed partner (for nocturnal events) – Sleep studies (polysomnography) |
| Treatment | – Cognitive-behavioral therapies – Medications (when necessary) – Lifestyle modifications | – Behavioral interventions (e.g., safety measures for sleepwalkers) – Medications (in some cases, for specific parasomnias) |
| Prevalence | Common, affecting a significant portion of the population | Less common, but prevalence varies by type of parasomnia |
| Long-Term Consequences | Increased risk of health issues (e.g., cardiovascular diseases, mood disorders) if left untreated | Potential safety risks, risk of injury during parasomnia episodes, and psychological distress if left untreated |
| Examples | – Primary insomnia – Secondary insomnia (due to underlying medical or psychiatric conditions) | – Sleepwalking (somnambulism) – Night terrors (sleep terrors) – REM behavior disorder (RBD) – Sleep-related eating disorder (SRED) – Sleep paralysis |
Please note that while this table provides a general comparison, individual experiences of insomnia and parasomnia can vary widely, and proper diagnosis and treatment should be based on a healthcare professional’s assessment.
Abnormal behaviors or experiences during sleep
The abnormal behaviors or experiences experienced that occur during sleep, usually related to parasomnia can refer to the activities such as movements, motions, or even events that happen while sleeping. These experiences and behaviors are considered to be unusual because they are different from the normal and normal patterns of sleep.
A few examples of strange behavior and experiences in sleep typically associated with sleep disorders like parasomnia include:
- Sleepwalking (Somnambulism): Sleepwalking is when a person gets out of bed and moves around in a state of sleep. The sleepwalker may engage in various activities, like walking around aimlessly, opening doors, or eating food, all while being in a state of partial arousal.
- night Terrors (Sleep Terrors): Night terrors are characterized by a sudden awakening from sleep, accompanied by intense anxiety, confusion and sometimes crying or screaming. The person who is experiencing an evening terror will usually be confused and might not recall the event when they awake.
- Sleep-talking (Somniloquy): Sleep-talking refers to speaking while asleep. This could range from basic murmurs that are unintelligible to more coherent conversations. Sleep talkers often are not aware that they are doing something wrong.
- REM behavior disorder (RBD): RBD is a disorder in which people physically act out their fantasies while in REM (rapid eye movements) sleep. It can be characterized by movements or vocalizations. It can also include violent or aggressive behavior while asleep.
- Sleep-Related Eating Disorder (SRED): Individuals who suffer from SRED consume food during their sleep typically consuming large amounts of food, but are not aware of what they are doing. They may not remember any of the eating incidents.
- Sleep Paralysis The condition of sleep paralysis can be described as a temporary impairment of movement or talk while asleep or awakening. It is often caused by vivid hallucinations or the sensation of intense tension or anxiety.
- Exploding Head syndrome (EHS): This phenomenon is caused by hearing explosive, loud noises or sensations, for example, a sudden, loud blast or electric shock during the transition from wakefulness to sleep.
- Sexsomnia The term “sexsomnia,” also called sleep sex is when you engage in sexual activities while asleep, with no conscious awareness. It can involve sexual contact or fondling, as well as sexual interactions.
It is important to recognize that the exact nature and intensity of the abnormal behavior or experiences in sleep may vary from person to person. Parasomnias can be caused by many triggers, like the genetics of the disorder, stress or sleep deprivation as well as other sleep disorders.
The diagnosis and treatment typically involve an evaluation by a medical professional that may include sleep tests (polysomnography) to observe the patterns of sleep and behavior.
Relationship and social consequences
Parasomnias, which are characterized by abnormal behavior or experiences during sleeping, can cause profound social and relational consequences for people who suffer from them. The consequences could affect the person suffering from the condition and their family members as well as the bed partner.
Here are some relational and social consequences that are associated with parasomnias:
- Safety Risks: Parasomnias could pose security risks for the person who suffers from parasomnia as well as those who are in the same sleep space. For example, sleepwalking and violent behavior that is related to REM behavior disorder (RBD) can result in injuries or accidents. Family members or friends might be concerned about the individual’s security and may take steps to protect themselves from harm.
- Disruption of a Bed Partner’s Sleep: The effects of insomnia can affect the sleep of bedmates. Sleep talking, night terrors, or violent movements during sleep can the person who shares a bed which can cause insomnia for both parties. In time, this may result in sleep loss and stress upon the bond.
- Communication Problems: Parasomnias may lead to communication issues in relationships. Sleep talkers might say phrases that can be disturbing or confusing to their sleeping partners. The attempts to communicate during a parasomnia-related episode might not be effective due to the person’s alteration in consciousness.
- Psychological Distress: Parasomnias can be a source of psychological distress for both the person suffering from the disorder and their family members. Being a witness to a loved one or family member experiencing sleepwalking or night terrors sleepwalking can be emotionally traumatic and cause anxiety or fear.
- Lower quality of sleep: Frequent disruptions caused by the parasomnia of a partner can lead to a reduction in the quality of sleep for both people. Lack of sleep can cause emotional disturbances, and mood swings and adversely affect the general health of those who are affected.
- The stress of relationships: Chronic and severe parasomnias can cause stress to relationships, especially when they aren’t properly controlled or understood. Disappointment, confusion, and conflict can arise because of parasomnia-related issues.
- Social Isolation: Parasomnia sufferers may feel isolated from others or reluctant to participate in evening events with their family or friends because of the anxiety of being embarrassed or disrupting events occurring in the presence of other people.
To tackle the social and relationship implications of sleep disorders, it is crucial for people who suffer from these sleep disorders to seek medical examination and treatment. A proper diagnosis and treatment can assist in reducing the impact of sleep disorders on relationships and enhance the standard of living for those affected as well as their loved ones.
Informing bed partners and family members of the symptoms of parasomnia will help to build trust and encourage assistance, leading to more effective strategies for dealing with the condition.
Association with stress and anxiety
The two sleep disorders are able to be linked to anxiety and stress, however, the specific nature of this connection can differ between these two sleep disorders.
- Insomnia and Stress/Anxiety:
- Causal Connection: Stress and anxiety are frequent triggers for short- or long-term sleepiness. Life events that stress you like work-related stressors relationships financial stressors, and traumatizing experiences, can result in increased arousal, and make it hard to sleep and relax.
- Chronic insomnia: Continuous experience of stress, or anxiety can lead to the creation the condition of chronic insomnia. In certain cases anxiety about not sleeping could trigger an unending cycle of anxiety and insomnia and the fear of insomnia can exacerbate the issue.
- Maintaining Factors: Anxiety and stress may be contributing factors to insomnia even after the initial stressor has been eliminated. People who have an insomnia history may have trouble sleeping due to increased vigilance or anxiety that is related to sleeping.
- Parasomnia and Stress/Anxiety:
- Triggers for Sleep Disorders: Stress and anxiety can trigger or intensify certain parasomnias, particularly those that manifest during sleep that is not REM, for example, sleepwalking or night terrors. Arousal of the emotional throughout the day can affect sleep-related behaviors.
- REM Behavior Disorder (RBD): Stress and anxiety are two factors that can cause REM Behavior Disorder (RBD) which is a condition where people act out their dreams in REM sleep. The emotional turmoil or the heightened states can trigger more intense enactment of dreams.
- Anxiety-inducing Parasomnias: Certain parasomnias, such as night terrors, can be more frequent in people who suffer from anxiety disorders. Anxiety and stress can trigger these types of events.
Stress and anxiety can contribute significantly to the onset, exacerbation, or maintenance of both insomnia and some parasomnias. The management of stress and anxiety via relaxation techniques, cognitive behavioral therapies, and lifestyle adjustments could be beneficial for those suffering from insomnia and sleep-related disorders.
Addressing the root factors that cause anxiety and stress, if relevant, can be an important aspect of treatment for sleep disorders and insomnia. Talking to a doctor or sleep specialist can assist individuals in coming up with effective strategies to deal with these sleep-related issues within the context of anxiety and stress.
Potential overlap in symptoms
There’s a possibility of an overlap in symptoms between parasomnia and insomnia that can make it difficult to distinguish between both sleep-related disorders.
Here are a few symptoms that could be overlapping:
- Sleep disturbance: Both insomnia and parasomnia are known to disrupt sleeping patterns, causing disturbances in sleep. Patients suffering from insomnia usually have trouble falling asleep, remaining asleep, or awakening early in the morning which can lead to uneven sleep. The parasomnia-related symptoms, such as sleepwalking or night terrors, can trigger sudden awakens and sleep disturbances.
- Daytime Fatigue: Fatigue during the day is a frequent complication of insomnia and parasomnia. Sleeplessness can cause lack, which can result in a decrease in sleepiness during the day, impaired cognitive function, as well as mood disorders. In the same way, parasomnia-related episodes may trigger awakenings in the night, which can lead to insomnia and fatigue during the day.
- Impaired concentration: Individuals with both parasomnia and insomnia may suffer reduced cognitive performance and decreased concentration due to sleep disturbances. Sleep deprivation caused by insomnia can cause difficulties with concentration, memory issues, and decreased alertness. The parasomnia episode can also cause problems with the functioning of your brain throughout the daytime.
- Disorders of Mood: Disorders of the mood such as irritability anxiety and mood swings can be experienced in sleep and insomnia. Chronic insomnia may contribute to mood disorders, and the stress that comes with parasomnias, particularly if they cause injuries or accidents, can affect mood.
- Sleep-related anxiety: Both of these conditions can cause anxiety that is related to sleep. Individuals suffering from insomnia can develop anxiety about being unable to sleep or remain asleep, which can lead to an increase in arousal and sleep problems. Patients who experience parasomnia attacks might also experience anxiety over sleep-related behaviors as well as the anticipation of episodes.
- Sleep Talking: Talking to yourself, which is a parasomnia-related symptom, may be confused with sleep-related rumination or even restlessness. Sleep talkers might use words or phrases in sleep, which can be confused as symptoms of insomnia.
- Trouble Recalling Sleep Events: Those suffering from parasomnia could be unable to recall the details of their nighttime routines or experiences, which can lead to confusion regarding the cause of their sleep disorders. This may be similar to the inability to remember certain types of insomnia.
It’s crucial to understand that even though there could be symptoms that overlap, an attentive examination by a medical professional or a sleep specialist, with a thorough log of sleep, a history as well and sleep studies, will aid in identifying insomnia from parasomnia.
A precise diagnosis is crucial for determining the most appropriate treatment and treatment options for these specific sleep conditions.
Similarities Between Insomnia and Parasomnia
Although they are distinct sleep disorders Parasomnia and insomnia share certain similarities, especially in the way they impact the quality of sleep for a person and their overall health.
Here are some similarities that they share:
- Sleep Disruption: Parasomnia and insomnia can alter normal sleeping patterns, causing difficulty in achieving restorative sleep. Insomnia is defined by problems sleeping and staying asleep, as well as awakenings in the early morning, which cause sleep disruptions. Parasomnias can cause abnormal behavior or sleep-related experiences that can result in sudden awakenings or disturbances in sleep.
- Daytime impairments: Individuals with both insomnia and parasomnia frequently experience problems during the daytime. Sleep deprivation caused by insomnia can cause fatigue, sleepiness during the day, and reduced alertness, as well as impaired cognition, and mood disorders. In the same way, sleep-related episodes may result in the daytime fatigue, sleepiness, and mood shifts.
- Psychology: Both disorders can result in psychological effects. Chronic insomnia is linked to an increased risk of developing mood disorders, including anxiety and depression and heightened levels of stress. Sleepiness, particularly if they are persistent or stressful, may result in psychological stress and anxiety.
- Qualities of life: Insomnia and parasomnia can have a negative impact on the quality of life for an individual. Sleep disturbances caused by any disorder can result in less overall well-being, lower productivity, as well as impaired performance in occupational and social settings.
- Possibility of comorbidity; Parasomnia and insomnia can occur in conjunction with sleep disorders that are not related to medical illnesses. For instance, people with parasomnias can also suffer from insomnia as a result of an increase in anxiety or increased arousal triggered by their parasomnia-related episodes.
- Stress and anxiety: Both disorders can be caused or worsened by anxiety and stress. Life events that stress you or cause anxiety may contribute to the inability to sleep or the recurrence of insomnia. Stress can cause or worsen certain sleep disorders like sleepwalking or night terrors.
- Impact on Relationships: Both conditions can affect relationships as sleep issues can impact bed partners as well as family members. Sleep disruption, whether caused by insomnia-related restlessness as well as the presence of episodes of sleep parasomnia can be a source of tension and cause conflicts.
- Achieving a Correct Diagnosis and Treatment: In both cases patients need a correct diagnosis and the appropriate treatment. A precise diagnosis by an expert in healthcare or a sleep specialist is necessary to identify the exact sleep disorder and create an effective treatment program that is customized to the individual’s requirements.
While there are some resemblances, however, there are some significant distinctions between parasomnia and insomnia and parasomnia, which include the causes symptoms, and treatment. A precise diagnosis is essential in order to ensure that people get the right treatment to address their specific sleep problems.
Reference Books
Certainly, here are some reference books on sleep disorders, insomnia, and related topics:
- “The Promise of Sleep: A Pioneer in Sleep Medicine Explores the Vital Connection Between Health, Happiness, and a Good Night’s Sleep” by William C. Dement and Christopher Vaughan
- This book provides a comprehensive overview of sleep, its importance, and various sleep disorders, including insomnia. It also offers insights into the latest research and treatments in the field of sleep medicine.
- “Insomnia: Principles and Management” by Christopher P. Morin and Charles M. Morin
- This authoritative book focuses specifically on insomnia, covering its diagnosis, assessment, and various treatment options, including cognitive-behavioral therapy for insomnia (CBT-I).
- “Principles and Practice of Sleep Medicine” edited by Meir H. Kryger, Thomas Roth, and William C. Dement
- This comprehensive textbook is a go-to reference for sleep medicine professionals. It covers a wide range of sleep disorders, including insomnia, parasomnias, and many others, providing in-depth information on diagnosis and treatment.
- “Atlas of Clinical Sleep Medicine” by Meir H. Kryger, Richard B. Berry, and Russell Rosenberg
- This atlas-style book includes visual aids and case studies, making it a valuable resource for healthcare professionals seeking to understand and diagnose sleep disorders, including insomnia and parasomnias.
- “The Sleep Solution: Why Your Sleep is Broken and How to Fix It” by W. Chris Winter, MD
- Written by a sleep specialist, this book offers practical advice on improving sleep quality and addressing sleep-related issues, including insomnia. It covers a wide range of sleep topics in an accessible manner.
- “Why We Sleep: Unlocking the Power of Sleep and Dreams” by Matthew Walker
- While not a clinical manual, this book explores the science of sleep, its significance, and the impact of sleep on our overall health and well-being. It provides valuable insights into the importance of addressing sleep disorders.
- “Clinical Handbook of Insomnia” edited by Hrayr P. Attarian
- This handbook is designed for clinicians and provides practical guidance on the diagnosis and management of insomnia. It includes information on various treatment modalities and approaches.
- “Sleep Disorders Medicine: Basic Science, Technical Considerations, and Clinical Aspects” edited by Sudhansu Chokroverty and Robert J. Thomas
- This comprehensive textbook covers a wide range of sleep disorders and their clinical aspects. It serves as a valuable resource for healthcare professionals and researchers in the field of sleep medicine.
Conclusion
Knowing the distinctions and similarities between parasomnia and insomnia is vital to successfully tackling sleep disorders. Although both disorders can affect sleep patterns and can have different effects on a person’s health They have distinct features in terms of causes, symptoms, and treatment methods.
A precise diagnosis by health experts is essential to providing the appropriate treatment and improving the quality of sleep, eventually leading to better overall health and a better quality of life.