Introduction
Thrombocytopenia and Thrombocytosis are medical conditions involving Abnormalities of platelet count. Platelets play a vital role in Hemostasis – the body’s natural ability to stop Bleeding by creating blood clots – by helping form them to Control bleeding.
Thrombocytopenia refers to a decrease in platelets below their normal range of 150,000-450,000 per microliter of blood due to factors like immune system disorders, infections, medications or bone marrow disorders; or certain medical treatments. It increases bleeding risk and causes bruises more readily than usual.
Thrombocytosis refers to an abnormally elevated level of platelets in the blood, exceeding normal limits. There are two forms of thrombocytosis: primary (essential thrombocythemia) and secondary thrombocytosis, with the former caused by genetic mutations while the latter can result from infections, inflammations, cancers or conditions that necessitate immune suppression such as HIV.
Understanding thrombocytopenia and thrombocytosis – their causes, symptoms, diagnosis and treatments – is critical to effective medical care and management.
Over the next several sections, we will examine thrombocytopenia and thrombocytosis in detail, exploring their definitions, causes, symptoms, diagnosis, potential treatments options and possible management approaches. By understanding these conditions in depth, individuals will be better equipped to recognize signs and seek medical help when necessary as well as take an active part in their healthcare management.
Definition of thrombocytopenia
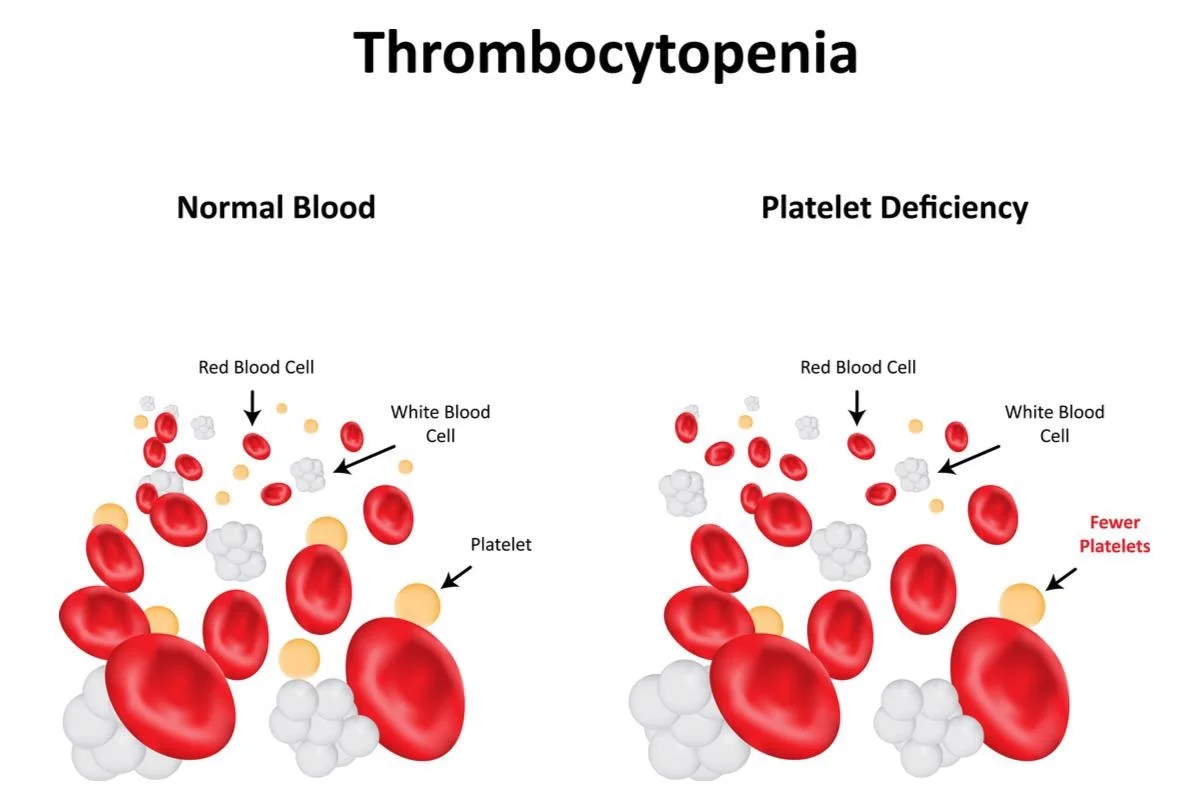
Thrombocytopenia is a Medical condition in which there is a Reduced number of platelets (also called Thrombocytes) in the blood. Platelets play a critical role in Blood clotting and Controlling Excessive bleeding, so their absence causes haemorrhages that require constant medical intervention to control.
Healthy Individuals typically have platelet counts ranging Between 150,000 and 450,000 platelets per Microliter of blood, but when their count drops below this Normal range it can make it more difficult for blood clots to form and prevent bleeding.
This Condition is known as Thrombocytopenia. Thrombocypenia can be caused by various underlying factors, including immune system disorders, infections, medications, bone marrow disorders and some medical treatments.
As the severity of Thrombocytopenia varies Greatly, those living with it may experience Symptoms including easy bruising and Petechiae (small red or purple spots on the skin), prolonged bleeding from cuts or injuries as well as frequent bruising and petechiae occurrence. Receiving prompt diagnosis and appropriate treatments are key in managing and treating this condition effectively.
Definition of thrombocytosis
Thrombocytosis is a Medical condition marked by an unusually high Concentration of platelets (thrombocytes) in the blood. Platelets play an integral part in blood clotting and their Primary purpose is preventing excessive bleeding; for Healthy individuals their normal platelet count typically ranges from 150,000-450,000 per microliter of blood; when this exceeds this upper limit it becomes thrombocytosis; there are two forms: primary (also known as essential thrombocythemia) and secondary thrombocytosis (both primary).
Primary thrombocytosis is a Myeloproliferative disorder Characterized by the abnormal overproduction of Platelets in bone marrow due to genetic mutations of cells Responsible for producing platelets. Secondary thrombocytosis occurs as a reactive condition when platelet counts increase due to infections, inflammations, certain cancers or iron deficiency states – or following surgical removal of the spleen.
Thrombocytosis may not manifest any noticeable symptoms and is discovered incidentally during routine blood tests, yet in other instances individuals living with thrombocytosis may experience headaches, dizziness and chest pain as symptoms of their disease. Furthermore, having thrombocytosis increases the risk of abnormal blood clot formation which may lead to complications like deep vein thrombosis or stroke.
Diagnosing thrombocytosis typically involves taking a complete blood count (CBC) test to measure platelet counts and additional investigations, particularly for secondary cases, to ascertain their causes. Treatment options depend on identifying these underlying causes: medication may be prescribed to decrease risk of clot formation in primary cases; treating secondary conditions or eliminating triggers can also help. It’s essential that regular monitoring and management occur for anyone suffering from thrombocytosis to avoid complications associated with it.
Comparison Table of Thrombocytopenia and Thrombocytosis
Below is a comparison table highlighting the key differences between thrombocytopenia and thrombocytosis:
| Aspect | Thrombocytopenia | Thrombocytosis |
|---|---|---|
| Definition | Decreased number of platelets in the blood | Increased number of platelets in the blood |
| Platelet Count | Below normal range (150,000 to 450,000 platelets per microliter of blood) | Above normal range (exceeding 450,000 platelets per microliter of blood) |
| Causes | Immune system disorders, infections, medications, bone marrow disorders, etc. | Infections, inflammation, certain cancers, chronic myeloproliferative disorders, etc. |
| Symptoms | Easy bruising, petechiae (small red or purple spots on the skin), prolonged bleeding from cuts or injuries | Increased risk of blood clot formation, headaches, dizziness, chest pain (in severe cases) |
| Diagnosis | Complete blood count (CBC) test, additional tests to determine underlying cause | Complete blood count (CBC) test, further tests to identify underlying cause |
| Treatment | Addressing underlying cause, medications to stimulate platelet production, blood transfusions (in severe cases) | Addressing underlying cause, medications to prevent blood clot formation, platelet-lowering treatments (in certain cases) |
It is important to note that this table provides a general overview of the differences between thrombocytopenia and thrombocytosis.
The actual presentation, causes, symptoms, and treatment options may vary depending on individual cases and underlying conditions.
Proper diagnosis and medical guidance are essential for accurate assessment and management of these conditions.
Prolonged bleeding from cuts or injuries
Prolonged Bleeding from cuts or injuries is one of the Hallmark symptoms of Thrombocytopenia, a condition marked by low platelet counts in the blood. Platelets play an Essential role in blood clotting; when their count drops Drastically, their ability to form clots and control bleeding becomes Compromised.
Even minor cuts or injuries in individuals with thrombocytopenia can cause extensive bleeding that takes longer to stop due to decreased platelet counts; there are simply not enough clotting factors available at the injury site for stable clot formation, leading to prolonged and potentially significant blood loss.
Noting the severity of bleeding symptoms varies with both individual and overall thrombocytopenia severity, as can their frequency or intensity. Some may only experience occasional or mild episodes, while others could experience more frequent or severe episodes.
If you suspect Thrombocytopenia or have Experienced prolonged bleeding, seeking medical advice Immediately to obtain an Accurate diagnosis and the Necessary treatment should be of Paramount importance.
Additional tests to determine the underlying cause
When diagnosing thrombocytopenia or thrombocytosis, additional tests may be needed to ascertain the underlying cause. Healthcare professionals use these additional tests to isolate what factors contributed to an abnormal platelet count.
Below are some common additional diagnostic tests:
Blood Smear Examinaion: A blood smear involves the examination of a small sample of blood under a microscope, to visually inspect platelets for any anomalies in their size, shape or distribution that might indicate potential causes of thrombocytopenia or thrombocytosis. This test provides healthcare providers with invaluable insight into potential causes.
Bone Marrow Aspiration and Biopsy: Sometimes a bone marrow aspiration and biopsy may be required in order to evaluate the bone marrow where platelets are produced. For this procedure, a sample is collected from hipbone or another site and then studied under a microscope for abnormalities or disorders that might impair platelet production. This procedure helps identify any abnormalities that impede their production as early as possible.
Coagulation Studies: Coagulation studies evaluate how well blood clots, measuring prothrombin time (PT), activated partial thromboplastin time (aPTT), and the international normalized ratio (INR). They measure various clotting factors while helping rule out other potential causes for abnormal platelet counts.
Serologic Tests: Serologic tests are designed to detect antibodies or markers associated with certain conditions that lead to thrombocytopenia or thrombocytosis, such as Lupus or HIV. Such testing could potentially determine if those disorders contribute to abnormalities in platelets.
Genetic Testing: When diagnosing primary thrombocytosis, genetic testing may be conducted to detect specific genetic mutations related to it; such as mutations in the Janus Kinase 2 (JAK2) gene. Such tests help confirm diagnosis and inform treatment decisions.
Noting the specific tests required depends upon an individual’s clinical presentation, medical history and suspected root causes of their condition. Healthcare professionals will consider these factors and order any additional necessary tests necessary for accurate diagnosis and developing an effective treatment plan.
Platelet-lowering treatments should only be considered in specific instances of thrombocytosis where p
Platelet-lowering treatments in certain cases
latelet counts are significantly elevated and there is an increased risk of abnormal blood clot formation, and they aim to bring platelets down into safer levels and thus lower risk.
When making this Decision, several factors should be Considered such as cause, Symptoms and overall health Conditions of an Individual as well as any current Medications for chronic illnesses like Thrombocytosis or Hypercoagulability (thrombocytosis, in this instance).
Here are some Commonly used platelet-lowering treatments:
Medication: Low-dose aspirin may be prescribed to inhibit platelet aggregation and lower the risk of blood clots. It’s often used in cases of essential or secondary thrombocythemia associated with certain myeloproliferative disorders.
Hydroxyurea: Hydroxyurea is a medication designed to suppress bone marrow production of platelets. It’s often prescribed in primary thrombocytosis cases – particularly essential thrombocythemia – in order to decrease platelet counts and avoid potential clotting complications.
Anagrelide: Anagrelide is another medication designed to lower platelet counts by suppressing their production, often used as a solution for essential thrombocythemia when other treatments prove ineffective or are unsuitable.
Plateletpheresis: Plateletpheresis is similar to plasma or blood donation in that blood is drawn from an individual and then platelets are isolated and removed, returning the remaining components (red blood cells and plasma).
Plateletpheresis provides immediate reduction of platelet counts; therefore it’s most frequently used during emergencies or severe cases of thrombocytosis with high risks of clotting.
Note that platelet-lowering treatments are not necessarily appropriate or necessary in all cases of thrombocytosis; rather, each individual must consider their underlying cause, health status, potential risks and benefits of intervention as they make this decision.
Healthcare providers will carefully evaluate each case in order to select an approach which will effectively manage thrombocytosis without associated complications.
Encouragement to seek medical attention for any abnormal bleeding or clotting symptoms
Attentiveness to any abnormal bleeding or clotting symptoms should always be prioritized, so when prolonged or unexplained bleeding from cuts or injuries occurs, frequent nosebleeds occur, or there are symptoms suggestive of blood clot formation (including chest pain, shortness of breath or sudden severe headaches ), it is imperative to seek medical assistance immediately.
Abnormal bleeding or clotting symptoms could be signs of an underlying condition like thrombocytopenia or thrombocytosis, which requires professional medical evaluation and management. Only healthcare providers can accurately assess symptoms, conduct relevant tests, and offer guidance and treatment accordingly.
Do not dismiss or minimize these symptoms as they could be signs of serious health conditions. Early medical intervention can prevent complications, treat the cause effectively and enhance overall well-being.
As always, your health should come first and seeking medical help should be considered an active step in understanding and treating any potential concerns. By advocating for yourself with healthcare providers to ensure the highest standard of care that leads to optimal results.
Conclusion
Thrombocytopenia and thrombocytosis are two distinct medical conditions involving abnormalities in platelet counts. Thrombocytopenia occurs when Platelet numbers fall below their normal range, Increasing risk of bleeding from cuts or injuries and Prolonging healing times. On the other hand, Thrombocytosis involves Elevated platelet counts beyond what would Normally be found, increasing risks of Abnormal blood clot formation and Prolonged healing from cuts or Injuries.
Thrombocytopenia may be caused by Immune system disorders, Infections, medications or bone Marrow disorders; while Thrombocytosis can either be genetic or secondary due to infections, Inflammation or cancer.