Pemphigus Vulgaris and Pemphigus Foliaceus are two autoimmune skin conditions that have blisters and are similar in their appearance however, they differ greatly in their characteristic clinical features, etiology, and treatment strategies. This outline of content aims to clarify the major distinctions between these disorders for a more accurate diagnosis and effective treatment.
Definition of Pemphigus Vulgaris
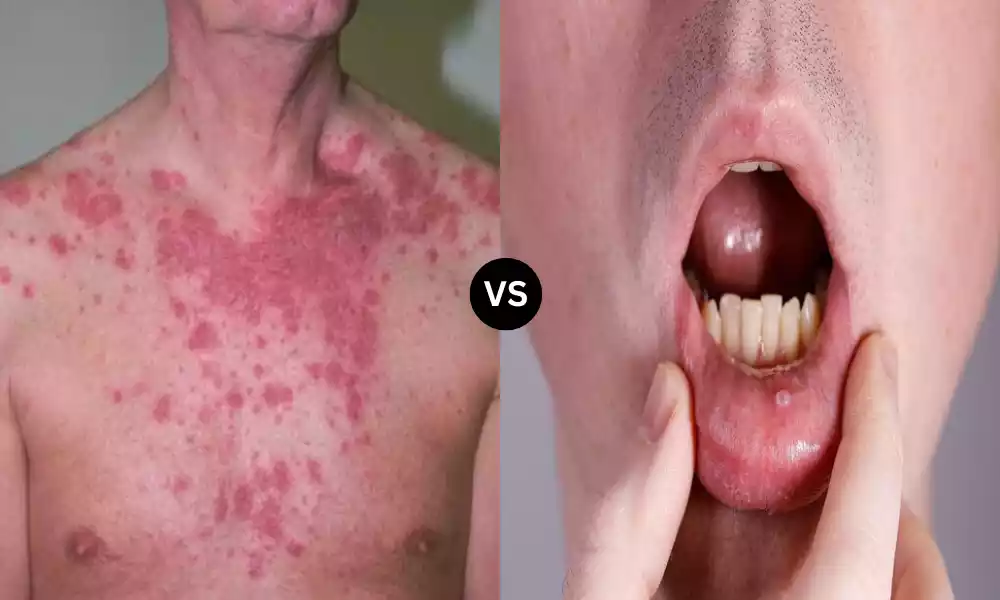
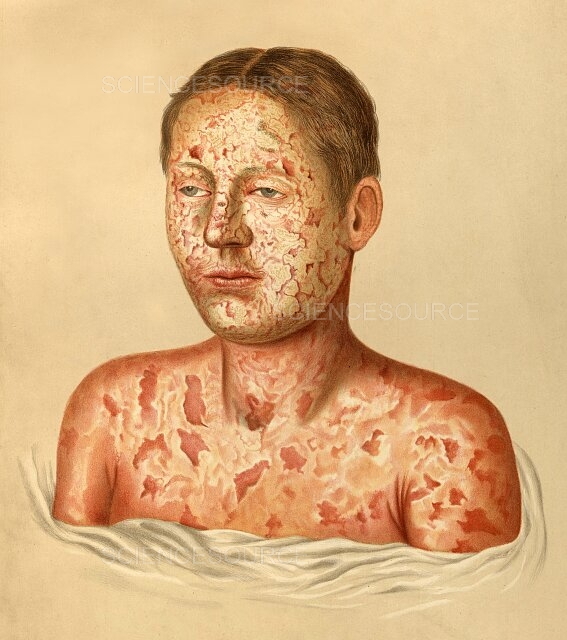
Pemphigus Vulgaris is a rare, severe autoimmune disease that manifests itself in the formation of painful liquid-filled, and swollen blisters (bullae) in the mucous membranes as well as the skin.
In this situation the immune system creates antibodies to attack and target desmoglein 3 which is a protein that is responsible for maintaining the skin’s integrity and mucosal tissue, leading to the destruction of adhesion to cells and the formation of extensive blisters.
Pemphigus Vulgaris most commonly affects the oral cavity, however, it can also affect the skin and mucous membranes. It could cause life-threatening complications if they are not recognized and addressed.
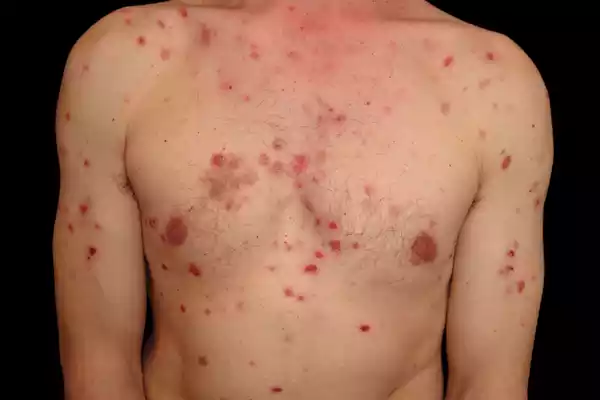
Definition of Pemphigus Foliaceus
Pemphigus Foliaceus can be described as an autoimmune skin disorder that is characterized by the development of small, fragile blisters on the uppermost layers (epidermis). In this situation, the immune system creates antibodies that attack and target desmoglein 1, which is a protein that is responsible for maintaining the skin cell’s adhesion.
The autoimmune reaction leads to the separation of skin cells from each other, resulting in scaly, crusted, and occasionally pruritic (itchy) spots on the skin’s surface. Contrary to Pemphigus Vulgaris Pemphigus Foliaceus mostly affects skin, and is less frequently connected with mucous membrane irritation, which makes it less severe.
Importance of distinguishing between Pemphigus Vulgaris and Pemphigus
Differentiating the difference between Pemphigus Vulgaris as well as Pemphigus Foliaceus is essential for a number of reasons:
- Treatment Choice: The treatment approaches for both conditions differ greatly. Pemphigus Vulgaris typically requires more intense immunosuppressive treatment because of its risk of serious mucosal involvement and potentially life-threatening complications. However, Pemphigus Foliaceus is typically less severe and could respond to less intensive treatment. A precise diagnosis will ensure you receive effective and efficient treatment, with a minimum of unwanted negative effects and costs for healthcare.
- Prognosis: Pemphigus Vulgaris has a higher likelihood of complications, and possibly a worse prognosis than Pemphigus Foliaceus. Knowing what variant the patient is suffering from can aid healthcare professionals in making more precise predictions of the course of the disease and possible results, which allows for better long-term treatment and counseling for patients.
- prevention of Complications: Both conditions may result in secondary infections due to skin lesions. Pemphigus Vulgaris has more of at chance of developing complications due to its involvement in the mucosal. An accurate diagnosis and the right treatment will reduce the chance of complications, such as sepsis and infections.
- Medication Choice: The choice of drugs, such as corticosteroids or immunosuppressants can differ according to the pemphigus-related variant. Making sure that the appropriate medication is used for the specific condition helps reduce adverse effects and improve the outcomes of treatment.
- Qualities of life: Pemphigus can have profound effects on a patient’s quality living, specifically in the areas of discomfort, pain, and emotional stress. Knowing the exact type of condition allows health professionals to customize the treatment plan and other supportive strategies to meet the specific difficulties faced by each patient.
- Research as well as Clinical Trials: Accurate diagnosis is crucial for enrolling participants in clinical trials as well as research studies. Making a distinction between the two conditions of Pemphigus Vulgaris from Pemphigus Foliaceus makes sure that patients are appropriately classified for research purposes, which leads to more accurate and reliable research findings.
Knowing the difference between Pemphigus Vulgaris from Pemphigus Foliaceus is vital for offering individualized treatment, maximizing the results of treatment, and improving the overall health of those suffering from the autoimmune skin conditions that cause blisters.
Comparison Table of Pemphigus Vulgaris and Pemphigus Foliaceus
Here’s a comparison table outlining the key differences between Pemphigus Vulgaris and Pemphigus Foliaceus:
| Characteristic | Pemphigus Vulgaris | Pemphigus foliaceus |
|---|---|---|
| Etiology | Autoimmune disorder | Autoimmune disorder |
| Target Antigen | Desmoglein 3 | Desmoglein 1 |
| Predominant Lesion Location | Mucous membranes, oral cavity, esophagus, and skin Potentially severe and life-threatening | Superficial skin layers, rarely mucous membranes Generally milder and less severe |
| Painful Blisters | Yes, painful blisters and mucosal erosions | Yes, blistering, but typically less painful than Pemphigus Vulgaris |
| Distribution | Mucosal and skin involvement, including the scalp | Predominantly cutaneous involvement, less mucosal involvement |
| Diagnostic Tests | Direct immunofluorescence (DIF) shows IgG deposits in the epidermis, and Indirect immunofluorescence (IIF) shows circulating autoantibodies, Histopathological examination of biopsied tissue | Direct immunofluorescence (DIF) shows IgG deposits in the epidermis, and Indirect immunofluorescence (IIF) shows circulating autoantibodies, Histopathological examination of biopsied tissue |
| Treatment | High-dose corticosteroids, immunosuppressive agents, monoclonal antibodies (e.g., rituximab) | High-dose corticosteroids, immunosuppressive agents, monoclonal antibodies (e.g., rituximab) |
| Prognosis | Potentially severe and life-threatening if untreated; improved with early diagnosis | Generally milder and more favorable |
| Complications | Secondary infections due to open lesions, medication side effects, psychological distress | Secondary infections due to open lesions, medication side effects, psychological distress |
Please note that while this table highlights the typical differences between Pemphigus Vulgaris and Pemphigus Foliaceus, individual cases may vary, and accurate diagnosis by a healthcare professional is essential for proper management.
What is pemphigus foliaceus also called?
Pemphigus Foliaceus can be known as “Foliaceous Pemphigus” or simply “PF” for short. Both terms are commonly used interchangeably to refer to the exact autoimmune skin condition that is characterized by superficial blisters as well as the treatment of desmoglein1 within the epidermis.
How do you diagnose pemphigus foliaceus?
A diagnosis for Pemphigus Foliaceus (PF) usually involves an amalgamation of clinical examination as well as laboratory tests and histopathological examination.
Here’s the procedure for how PF will be identified:
- Clinical Exam: A dermatologist or medical professional will conduct an extensive physical exam and pay close attention to what appears to be skin lesions. If it is Pemphigus Foliaceus, they’ll be looking for signs that are characteristic such as superficial blisters scaled lesions, and crusts.
- Biopsy: Skin biopsy is typically used in order to verify the diagnosis. When a biopsy is performed the small portion of the affected skin is removed and then sent to a pathologist for analysis. If there is PF the biopsy will show specific histopathological characteristics, such as the presence of acantholysis (loss of cell-to-cell adhesion Keratinocytes) within the epidermal layers.
- Direct Immunofluorescence (DIF): DIF is a lab test that requires the examination of samples of skin under an ultraviolet microscope. For Pemphigus Foliaceus, this test usually will reveal IgG deposits in the epidermis’s upper layer, which suggests an immune response against desmoglein 1.
- IIF (IIF): Blood tests are conducted to identify circulating autoantibodies within the bloodstream of a patient. IIF is one of the tests that can determine the presence of autoantibodies that target desmoglein 1. Increased levels of antibodies in blood may support the diagnosis.
- Clinical Description: The clinical presentation which includes the kind and location of skin lesions can give valuable clues to diagnose. Pemphigus Foliaceus mostly affects the skin, with only a little mucous membrane involvement. This distinguishes it from other variants of pemphigus.
- Exclusion of other conditions: To make a definitive diagnosis of Pemphigus foliaceus, the other conditions that cause autoimmune blisters and skin disorders with similar symptoms must be eliminated through an examination of the patient, histopathology, and lab tests.
It is important to remember it is important to note that the condition Pemphigus foliaceus is an uncommon condition and a correct diagnosis requires knowledge in immunology and dermatology.
Thus, those who suspect having PF should seek a medical evaluation for diagnosis and evaluation by a medical specialist who is experienced in the management of conditions that cause autoimmune blisters. A timely proper diagnosis and a precise one is essential in initiating the proper treatment and improving outcomes for those suffering from Pemphigus Foliaceus.
What is the primary lesion of pemphigus foliaceus?
The most common lesions of Pemphigus Foliaceus (PF) can be usually a small pustule or blister at the surface of your skin. The blisters are usually fragile and can easily break which can lead to the development of crusted and eroded lesions. Contrary to other types of pemphigus Pemphigus Foliaceus mostly affects the topmost layer of the epidermis. These layers comprise Keratinocytes.
The most important characteristics of principal lesions in PF are:
- superficial blisters: Blisters of PF are found in the epidermis, specifically, in the upper layers. They are commonly referred to as “subcorneal” because they form in the middle of the outer layers of the surface (stratum corneum).
- Crested Lesions: After the blisters have ruptured and begin to crust, they can form over. The crusts may appear honey-colored or yellowish and could be surrounded by erosions.
- Scaling: The skin’s scaling process is typical in PF and is particularly noticeable around the crusted and blistered regions.
- Minimum Mucous Membrane Involvement: Unlike Pemphigus Vulgaris it is a common condition affecting the mucous membranes (such as the throat and mouth) The majority of the time, PF affects the skin, with only a little mucosal involvement.
It is important to remember that the symptoms of the condition Pemphigus Foliaceus may differ across people as well and the intensity of the symptoms can vary. The diagnosis and treatment should be carried out by a dermatologist or a healthcare professional who has experience dealing with conditions that cause autoimmune blisters to ensure an accurate diagnosis and treatment that is appropriate.
Similarities Between Pemphigus Vulgaris and Pemphigus Foliaceus
Pemphigus Vulgaris (PV) and Pemphigus Foliaceus (PF) are both skin conditions that cause autoimmune blisters While they share many differences, they have a few similarities:
- Autoimmune Origin: Both PF and PV are autoimmune diseases, which means they are the result of an ineffective immune system. In both cases the immune system creates antibodies to are directed at specific proteins in the skin, resulting in the formation of blisters.
- The epidermal targets: In both PV and PF the primary goal of an autoimmune attack is a particular desmosomal protein. The PV protein of interest is desmoglein 3 while in PF, it’s desmoglein 1. Both proteins play a crucial role in sustaining an adhesion between skin cells to the epidermis.
- Bullae Form: Both conditions are marked by the formation of blisters filled with fluid (bullae) in the face. The blisters are caused by the loss of adhesion cell-to-cell between epidermis keratinocytes.
- Superficial Skin Activation: Although PV can affect mucous membranes as well as skin The majority of the time, PF affects the skin. In both instances, the skin blisters are located in the epidermis’s upper layer which makes it a superficial condition of blistering.
- Like Diagnostic Tests: The diagnosis for both conditions is similar to tests in the laboratory like indirect immunofluorescence (DIF) and indirect immunofluorescence (IIF). DIF typically detects IgG deposits within the epidermis. IIF can detect the presence of autoantibodies in circulation.
- Autoantibodies: For both PF as well as PV, the autoantibodies develop against desmosomal proteins that are specific to them, which can cause disruption of cell adhesion as well as the formation of blisters. In PV, autoantibodies target desmoglein3 and in PF, they target desmoglein 1.
- Therapeutic Methods: Although the treatment strategies can differ in their intensity, both diseases are controlled by immunosuppressive therapy. Corticosteroids with high doses as well as other immunosuppressive drugs are often used to treat both PF and PV.
Although these are some similarities it’s important to note that there are some important distinctions among Pemphigus Vulgaris as well as Pemphigus Foliaceus, particularly in their clinical presentation as well as their severity and involvement of the mucous membrane. A precise diagnosis and a customized treatment is essential to manage these disorders effectively.
Reference Books
Certainly! Here are some reference books related to various subjects that you might find useful:
- Medicine and Healthcare:
- “Harrison’s Principles of Internal Medicine” by Dan Longo, Anthony Fauci, et al.
- “Robbins and Cotran Pathologic Basis of Disease” by Vinay Kumar, Abul K. Abbas, and Jon C. Aster.
- “Gray’s Anatomy for Students” by Richard Drake, A. Wayne Vogl, and Adam W.M. Mitchell.
- Psychology:
- “Psychology” by Saundra K. Ciccarelli and J. Noland White.
- “Abnormal Psychology” by Ronald J. Comer.
- “The Psychology Book” by DK.
- Computer Science and Programming:
- “Introduction to the Theory of Computation” by Michael Sipser.
- “Clean Code: A Handbook of Agile Software Craftsmanship” by Robert C. Martin.
- “Python Crash Course” by Eric Matthes.
- Science and Popular Science:
- “Cosmos” by Carl Sagan.
- “A Short History of Nearly Everything” by Bill Bryson.
- “Sapiens: A Brief History of Humankind” by Yuval Noah Harari.
- History:
- “A People’s History of the United States” by Howard Zinn.
- “The Guns of August” by Barbara W. Tuchman.
- “The Rise and Fall of the Third Reich” by William L. Shirer.
Conclusion
reference books are excellent sources for gaining knowledge, exploring new topics, and expanding our knowledge about the globe. No matter if you’re looking for information in psychology, medicine computers, or other area, a reference book is an authoritative guide.
The study and understanding of these books can help broaden your perspective spark curiosity and provide invaluable insights to help you grow professionally and personally. Also, whether you’re diving into the deepest depths of science, history as well as literature, or seeking advice on how to do things these reference books are essential guides on your journey to continuous learning.