Arthritis and Osteoarthritis are two musculoskeletal disorders that affect millions of people around the world. Although they have a lot in common with joint discomfort and pain they differ with regard to their causes, signs, and treatment strategies.
The main differences between osteoarthritis and arthritis offer valuable information to help patients and healthcare professionals know and manage these ailments.
Explanation of arthritis
Arthritis is a medical term used to describe inflammation of one or more joints within the body. It encompasses more than 100 distinct kinds of joint disorders and conditions that cause joint stiffness, pain, swelling, and reduced mobility.
Arthritis is a problem that affects individuals of all ages and backgrounds and the severity of it may range from minor irritation to long-term and debilitating joint injuries. The kind of arthritis, like osteoarthritis or rheumatoid arthritis, is what determines the root cause as well as symptoms and the treatment options available.
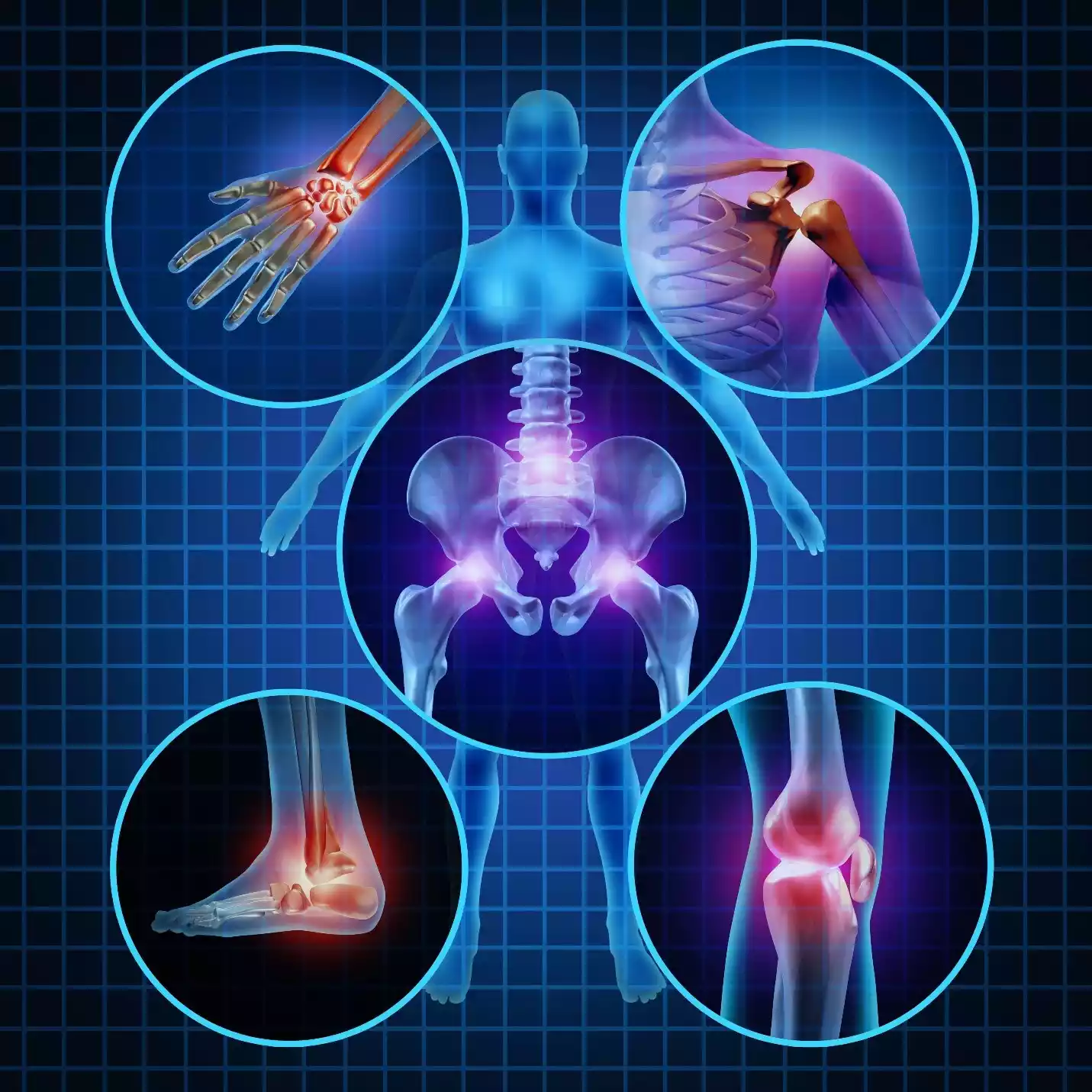
Explanation of osteoarthritis
Osteoarthritis often abbreviated as OA is a frequent degenerative joint condition characterized by the gradual loss of the protective cartilage which protects the bones’ ends in joints.
It is a type of arthritis that is mostly caused by age, wear and tear on joints, as well as, in certain cases joint injuries or genetic causes. When cartilage begins to degrade in time, it may cause stiffness, joint pain, inflammation, as well as a decrease in flexibility.
Osteoarthritis typically affects weight-bearing joints, such as the knees spine, hips, and hands. This condition is long-lasting and progressive. Its treatment typically consists of the relief of pain, lifestyle changes, and, in more severe cases, surgical procedures such as joint replacement.
Importance difference between Arthritis and Osteoarthritis
The most significant differences between osteoarthritis and arthritis lie in their underlying causes, mechanisms, and consequences for treatment and treatment. Knowing these distinctions is vital to make sure you get a precise diagnosis and provide effective treatment.
Here are the main distinctions:
- Etiology:
- Arthritis: Arthritis is a broad term that encompasses a variety of types of joint pain. It may be caused by an autoimmune disease (e.g. the rheumatoid joint) or infections, as well as other factors that affect the system.
- Osteoarthritis: Osteoarthritis is mostly a degenerative disorder caused by the gradual degradation of the joint cartilage. It’s often linked to age, mechanical stress or joint trauma.
- Inflammatory Response:
- Arthritis: The most common cause of arthritis is general inflammation that affects not just joints, but other body parts as well.
- Osteoarthritis: Osteoarthritis is defined by localized inflammation, which is usually more mild and restricted to the joint affected.
- Affected Joints:
- Arthritis: Arthritis can affect several joints in the body including large and small joints.
- Osteoarthritis: Osteoarthritis is a condition that affects specific joints, mainly weight bearing ones like hips, knees and spine.
- Age of Onset:
- Arthritis: Arthritis may occur at any age, and even for children (e.g. juvenile Idiopathic arthritis).
- Osteoarthritis: Osteoarthritis is more often linked with aging, with the risk rising as people age.
- Symptoms:
- Arthritis Arthritis symptoms can include joint stiffness, pain, swelling fatigue, and other general symptoms such as weight loss and fever, according to the type of arthritis.
- Osteoarthritis: Osteoarthritis is characterized by stiffness, joint pain, and decreased mobility in the joint that is affected.
- Progression:
- Arthritis: The course of arthritis can be a variety according to the root reason, but it can also be swift and cause joint deformity and disability.
- Osteoarthritis: Osteoarthritis tends to progress slowly with time, and is accompanied by the gradual loss of cartilage and changes in joint.
- Radiographic Differences:
- Arthritis: X-rays typically show joint space expanding and swelling of soft tissue in joints that are arthritic.
- Osteoarthritis: X-rays show the joint space shrinking osteophytes (bone spurs) as well as different structural shifts.
- Treatment Approaches:
- Arthritis: Treatment for arthritis usually includes medications to control immune and inflammation as well as disease-modifying medications, and lifestyle changes.
- Osteoarthritis: The treatment of osteoarthritis is based on exercises, pain relief, and weight control, as well as in extreme instances, surgical procedures like joint replacement.
- Prognosis:
- Arthritis: The prognosis of arthritis is largely dependent on the type of arthritis that it is, the severity of the condition, and the efficacy of treatment.
- Osteoarthritis: Osteoarthritis is usually a chronic illness that gets worse with time, however, it is usually manageable to preserve a good level of living.
Knowing the basic distinctions between osteoarthritis and arthritis is essential for healthcare professionals to offer proper care, and for patients to make informed choices about the treatment options and methods of management.
Comparison Table of Arthritis and Osteoarthritis
Here’s a simplified comparison table of arthritis and osteoarthritis:
| Aspect | Arthritis | Osteoarthritis |
|---|---|---|
| Definition | Inflammation of one or more joints | Degeneration of joint cartilage |
| Common Types | Rheumatoid arthritis, gout, etc. | Typically osteoarthritis |
| Causes | Autoimmune, infection, genetic | Aging, wear-and-tear, genetics |
| Affected Joints | Multiple joints are often involved | Specific joints, commonly weight-bearing |
| Age of Onset | Can occur at any age | More common with aging |
| Inflammatory Response | Systemic inflammation | Localized inflammation (mild) |
| Symptoms | Joint pain, swelling, stiffness | Joint pain, stiffness, reduced mobility |
| Progression | May progress rapidly | Typically progresses slowly |
| Radiographic Changes | Joint erosions, damage | Joint space narrowing, osteophytes |
| Diagnosis | Physical exam, blood tests, imaging | Physical exam, X-rays, MRI, etc. |
| Treatment | Medications, lifestyle changes | Medications, exercise, surgery |
| Prognosis | Variable can be severe | Generally chronic, worsens over time |
Please note that while this table provides a simplified comparison, both arthritis and osteoarthritis encompass various subtypes and individual variations in symptoms and severity.
Treatment approaches may also vary based on specific circumstances and the type of arthritis involved. Always consult a healthcare professional for accurate diagnosis and personalized guidance.
Wear-and-tear nature of osteoarthritis
Osteoarthritis (OA) can be typically described through its “wear-and-tear” nature because it is primarily caused by the progressive breakdown and degeneration of joint cartilage over the course of time.
Let’s take a closer review of this aspect of osteoarthritis:
- Cartilage degeneration: In joints that are healthy there is a smooth and secure layer of cartilage is encased over the bones’ ends. The cartilage allows bones to glide easily against each other in movements. In the case of osteoarthritis, this cartilage begins to wear away because of a variety of factors that include mechanical strain, aging-related changes, as well as genetic predisposition.
- Mechanical Stress: Osteoarthritis is a common condition that affects joints that are able to bear weight such as hips, knees, and the spine. These joints undergo substantial mechanical stress over their time. Things like running or lifting objects that weigh a lot or repetitive movements can result in wear and tear to the joints’ surfaces. The constant stress may accelerate the degeneration of cartilage.
- Age-related changes: As we age the cartilage of our bodies naturally loses its resilience and is less able to repair itself. The aging process causes the joint to be more prone to deterioration and less capable of maintaining the health of cartilage.
- Genetics: Certain people are genetically predisposed to develop osteoarthritis. Certain genetic influences can affect the structure and strength of joint cartilage. This makes them more prone to tear and wear.
- Joint injuries: Joint Injuries: Previous joint injuries like fractures, ligament tears, or dislocations may increase the chance of developing osteoarthritis. These injuries can affect the normal biomechanics and mechanics of the joint which can lead to sloppy wear of cartilage.
- Inflammatory response: While osteoarthritis can be generally regarded as a non-inflammatory disorder some researchers believe that a low level of inflammation in the joint might be a factor in cartilage loss and may contribute to an aging process.
- Other Factors: Obesity, inadequate joint alignment, as well as muscle weakness, may cause the joint’s mechanical stress which can increase wear and tear.
- Progress: As cartilage loses its elasticity bones can become closer and rub against one another. This can cause stiffness, pain as well as a decreased mobility. The body could try to heal the cartilage that has been damaged which can lead to the development of bone spurs (osteophytes) within the joint, which contribute to the wear-and-tear process.
It’s crucial to understand that osteoarthritis is a multifaceted disease with multiple causes, and the wear-and-tear aspect is only one aspect of the process of its development.
The treatment of osteoarthritis generally includes reduction in pain, lifestyle adjustments, and procedures to stop the progression of joint injuries and joint pain, with the aim of improving health and joint function.
Osteoarthritis has localized inflammation
Osteoarthritis (OA) is usually classified as an uninflammatory condition and any inflammation that is associated with it tends to be smaller and less severe in comparison to other types of arthritis, including Rheumatoid arthritis.
Here’s a more thorough explanation:
- Localized inflammation: In OA the majority of inflammation occurs in the joint affected. The inflammation is usually marked by slight swelling, redness, and a heightened temperature within the joint. The localized inflammation is due to the destruction and degeneration of cartilage in joints. It could result in the release of inflammatory chemicals as well as enzymes from the joint space.
- Synovitis: A few people with OA might suffer from a condition known as synovitis. It is a swelling of the synovial membrane, which is the part of the joint capsule that is lining it. Synovitis is a cause of localized joint inflammation, however, it’s not usually nearly as serious as general inflammation in inflammatory arthritis such as Rheumatoid arthritis.
- inflammatory mediators: In osteoarthritis, inflammatory mediators like prostaglandins and cytokines are created within the joint. These compounds can cause discomfort and damage to cartilage. However, the inflammation associated with OA is thought to be due to cartilage loss but isn’t the main cause of the disease since it’s a part of inflammation arthritis.
- Contrasts with the condition of Inflammatory Arthritis: In contrast to inflammatory arthritis such as rheumatoid arthritis in which an immune system attacks joints, causing general inflammation throughout the entire body the inflammation of OA is usually restricted to the joint affected and does not trigger an autoimmune reaction.
- Signs and symptoms: Localized inflammation that occurs in OA can cause symptoms like stiffness, joint pain, and swelling. This is particularly evident after prolonged periods of joint usage or physical exercise.
It’s crucial to realize that, while there’s some form of inflammation that is associated with OA however, it’s not characterized by the severe and widespread inflammation that is seen in other forms of arthritis.
The primary cause for osteoarthritis progression is the progressive destruction of joint cartilage typically due to factors such as mechanical stress, aging, or genetic predisposition.
Treatment of OA generally is focused on alleviating pain, lifestyle modifications, and treatments to limit further joint injury and inflammation in the joint affected.
Osteoarthritis symptoms are localized
Osteoarthritis (OA) signs tend to be restricted to the joints or joints. Contrary to other forms of arthritis, for instance, rheumatoid arthritis which may be characterized by systemic symptoms that affect many joints as well as other areas within the human body OA signs are usually restricted to the joints affected by the disease.
The most frequent localized symptoms of osteoarthritis comprise:
- Joint pain: The pain is one of the main signs of OA. It’s usually described as a numb and aching pain located in the joint that is affected. The pain can get worse when joint activity or use and it may ease with rest.
- Stiffness: Those suffering from OA frequently suffer from stiffness in the joint that is affected, particularly in the mornings or after long periods of inactivity. This stiffness may cause difficulty in moving the joint with ease.
- Reduced range of motion: OA can lead to a reduced range of motion within the joint affected. It can be difficult to bend, straighten, or turn the joint as normal.
- Swelling: The presence of localized swelling, also known as joint effusions can be seen in OA. The swelling is typically mild and results from the joint’s reaction to inflammation or irritation.
- Crepitus: Crepitus is the sensation of popping or crackling or sound inside the joint affected when it moves. It is a typical feeling in OA joints because of modifications in the joint’s structure.
- The weakness: As time passes muscle weakening can occur around the joint affected and can cause functional limitations.
- Tenderness: The joint might feel tender particularly if it’s constantly inflamed or irritated.
It is important to remember that the intensity of the localized symptoms can differ greatly between people and can also depend on the severity of osteoarthritis as well as the joints affected. Although osteoarthritis is primarily affecting the joints, it can also have an impact on general health and activities.
Management and treatment strategies for OA are usually focused on reducing localized symptoms as well as improving joint function and improving overall health.
Similarities Between Arthritis and Osteoarthritis
Osteoarthritis and arthritis share a number of similarities since both are characterized by joint-related issues. It is important to remember it’s a general term that covers different joint conditions, whereas osteoarthritis is one specific form of arthritis.
There are some similarities between the two:
- Joint Involvement: The two conditions of osteoarthritis and arthritis affect joints throughout the body, which can cause signs like stiffness, joint pain, and a decrease in mobility.
- Pain: joint pain is a common manifestation of both conditions. People suffering from osteoarthritis or arthritis often feel discomfort in joints affected by the.
- Stiffness: Stiffness of joints is a frequent complaint for both conditions particularly in the early mornings and after prolonged long periods of rest.
- Restricted range of motion: Osteoarthritis and arthritis can cause a restricted movement range in joints, which makes it difficult to do certain moves.
- Age-related risk: The fact is that arthritis can happen at any time but both diseases are more common as people age. The age of an individual is a major risk factor in the formation of osteoarthritis.
- X-ray findings: Imaging with radiography such as X-rays could reveal joint changes that are associated with osteoarthritis as well as arthritis well as the narrowing of joint spaces and bone spurs (osteophytes) and changes to the bone structure.
- Impact on daily life: The two conditions could significantly impact an individual’s life daily and general quality of life, especially when the symptoms are severe.
- Treatment Methodologies: The specific treatment will differ depending on the kind of arthritis, a variety of management methods for treating osteoarthritis and arthritis are compatible. They could include exercise, pain management physical therapy, and lifestyle changes.
- Chronic nature: Arthritis and osteoarthritis are usually chronic conditions that require long-term treatment and treatment. They can experience periods of symptom exacerbation or remission.
- Effect on joints: As time passes both ailments can cause joint injuries and, in more severe instances joint deformity. It can impact an individual’s ability to do routine activities and can lead to an impairment in standard of living.
It’s crucial to remember that although there are some differences, there are important differences between the various kinds of arthritis, such as Psoriatic arthritis, rheumatoid arthritis, and osteoarthritis.
A precise diagnosis by a doctor is vital to determining the type of arthritis and creating an appropriate treatment program that is customized to the individual’s requirements.
Reference Books
Certainly! Here are some reference books on a variety of topics that can provide valuable information and insights:
- Medicine and Health:
- “Harrison’s Principles of Internal Medicine” by Dennis L. Kasper et al.
- “The Merck Manual of Diagnosis and Therapy” by Robert S. Porter et al.
- “Gray’s Anatomy” by Henry Gray
- Science and Nature:
- “Cosmos” by Carl Sagan
- “A Short History of Nearly Everything” by Bill Bryson
- “Sapiens: A Brief History of Humankind” by Yuval Noah Harari
- History:
- “A People’s History of the United States” by Howard Zinn
- “Guns, Germs, and Steel: The Fates of Human Societies” by Jared Diamond
- “The Silk Roads: A New History of the World” by Peter Frankopan
- Philosophy:
- “Meditations” by Marcus Aurelius
- “The Republic” by Plato
- “Critique of Pure Reason” by Immanuel Kant
- Literature:
- “To Kill a Mockingbird” by Harper Lee
- “1984” by George Orwell
- “Pride and Prejudice” by Jane Austen
- Psychology:
- “Thinking, Fast and Slow” by Daniel Kahneman
- “The Man Who Mistook His Wife for a Hat” by Oliver Sacks
- “Influence: The Psychology of Persuasion” by Robert B. Cialdini
Conclusion
Reference books are vital sourcebooks that give you insight, knowledge, and perspectives on a broad range of topics that range from literature to medicine as well as history and psychology.
They function as guides and sources of information and a window into the world’s wisdom. If you are looking to increase your knowledge, expand your perspectives, or just indulge your curiosity appropriate reference book is a reliable companion in the process of learning throughout your life.
Therefore, grab an e-book, delve into the pages, and go on a journey to discover and learn.