Pemphigoid and Pemphigus are two distinct autoimmune skin conditions that affect the mucous membranes and skin. While they have a few similarities understanding the key differences is vital to ensure accurate diagnosis and the appropriate treatment. we will look at the features, diagnostics treatments, and key distinctions between pemphigus and pemphigoid and provide valuable insight into these difficult conditions.
What is Pemphigoid?
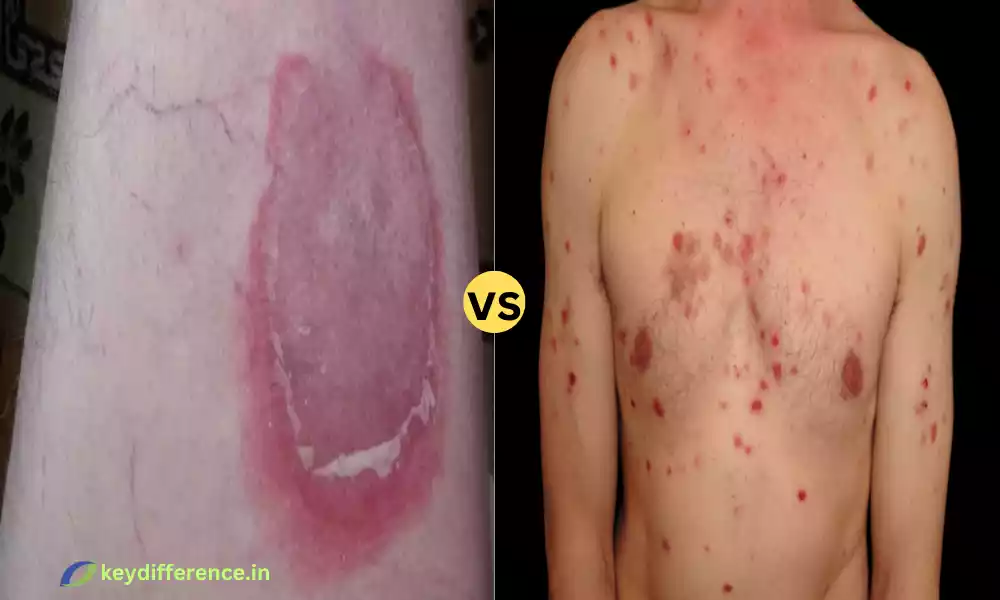
Pemphigoid is one of the rare autoimmune disorders that are characterized by the development of massive, tight, and swollen blisters on the mucous membranes and skin. These blisters are an outcome of the immune system attacking the proteins that hold the skin layers and mucous membranes.
The condition is most commonly seen in older people and may cause painful skin ulcers and irritations and is a serious dermatological problem that needs timely evaluation and therapy.
What is Pemphigus?
Pemphigus is among the rare autoimmune skin conditions that are marked by the formation of fluid-filled, fragile blisters on the mucous membranes of the skin. In pemphigus, it is when the immune system creates antibodies that attack and target certain proteins known as desmogleins which hold cell membranes of the skin together.
This causes connective tissue between the skin cells to be damaged, which leads to the development of blisters and the eroding of skin cells. Pemphigus can appear in many types, with pemphigus vulgaris and pemphigus foliaceous being the most frequent forms. The condition can be serious and life-threatening if appropriately treated.
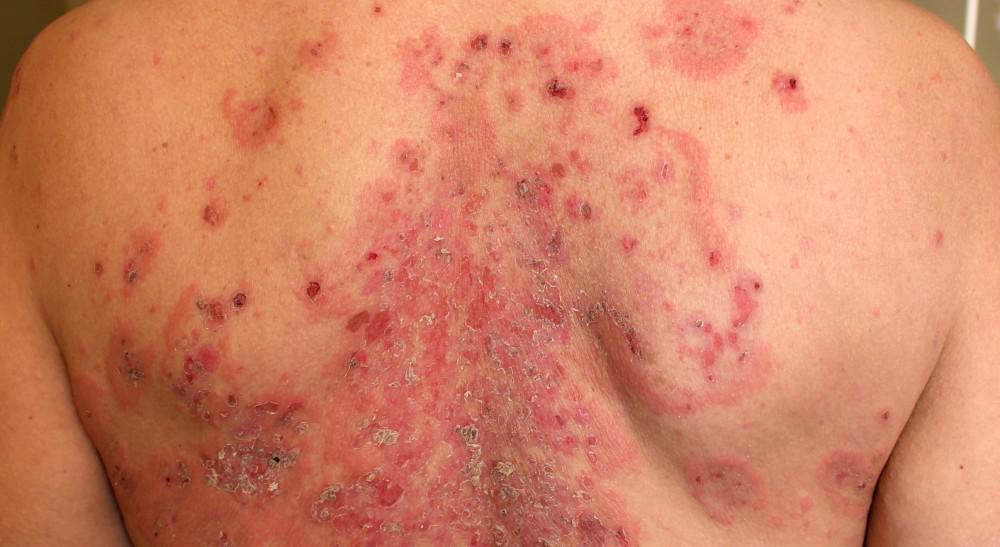
Comparison Table of Pemphigoid and Pemphigus
Here’s a comparison table highlighting the key differences between Pemphigoid and Pemphigus:
| Characteristic | Pemphigoid | Pemphigus |
|---|---|---|
| Definition | Autoimmune blistering disease | Autoimmune blistering disease |
| Types | Bullous Pemphigoid, Cicatricial Pemphigoid | Pemphigus Vulgaris, Pemphigus Foliaceus, Paraneoplastic Pemphigus |
| Autoantigens | BP180, BP230, or other basement membrane proteins | Desmoglein 1 (Dsg1) and Desmoglein 3 (Dsg3) |
| Target Tissues | Skin and mucous membranes | Skin and mucous membranes |
| Age of Onset | Typically older adults | Can affect a wide age range |
| Clinical Features | Large, tense blisters, and mucosal involvement common | Fragile blisters, and mucosal involvement common |
| Diagnosis | Clinical evaluation, biopsy, immunofluorescence tests | Clinical evaluation, biopsy, immunofluorescence tests |
| Disease Progression | Gradual, chronic course | Variable may have acute or chronic forms |
| Prognosis | Generally better prognosis than pemphigus | Prognosis can be more unpredictable and severe forms may be life-threatening |
| Treatment | Medications (e.g., corticosteroids, immunosuppressants) | Medications (e.g., corticosteroids, immunosuppressants), rituximab, IVIG |
| Common Types of Pemphigus | N/A | Pemphigus Vulgaris and Pemphigus Foliaceus are the most common forms |
| Key Autoantibodies | Anti-BP180 antibodies | Anti-desmoglein antibodies (anti-Dsg1 and anti-Dsg3) |
| Severity | Can be severe, but typically less severe than pemphigus | Can range from mild to severe, potentially life-threatening |
Please note that while this table outlines the primary differences between pemphigoid and pemphigus, each individual case can vary in terms of severity, response to treatment, and other factors. It is crucial for individuals with symptoms resembling these conditions to seek medical evaluation and diagnosis for appropriate care.
The importance of distinguishing between Pemphigoid and Pemphigus
Differentiating between pemphigus and psoriasis is crucial in both clinical practice and patient care because of numerous reasons that are crucial:
- Treatment Methodology: The distinction between the two autoimmune diseases is crucial as their treatment options differ dramatically. Pemphigoid generally responds well to specific medications such as corticosteroids as well as immunosuppressants. However, pemphigus might require different treatments including rituximab, or intravenous immunoglobulins (IVIG). Implementing the right treatment is essential to effectively controlling the disease and reducing the negative consequences.
- Prognosis: Knowing if the patient is suffering from pemphigoid or pemphigus is essential for understanding the course of the disease. Pemphigus could have a more uncertain and life-threatening course however, pemphigoid usually has better prospects for long-term survival. A precise diagnosis can help provide patients and their families with realistic expectations of the course of their disease and possible results.
- Preventing complications: Early diagnosis and appropriate treatment can prevent the complications that come with these illnesses. A delay or misdiagnosis can result in the development of severe mucosal and skin lesions, secondary infection, and a decrease in the quality of your life. The prompt treatment of the condition can decrease the chance of developing these conditions.
- Side Effects of Medication: Pemphigoids as well as pemphigus require ongoing medication management. Making sure you are taking the right medication specifically for the condition only enhances the efficacy of treatment but also minimizes potential adverse reactions and side effects related to these drugs.
- Quality of Quality of: Patients with chronic autoimmune blistering disorders often suffer from discomfort, pain, and diminished quality of life as a result of mucosal and skin lesions. An accurate diagnosis can ensure your patients get the effective and appropriate treatment, leading to a better management of symptoms and better health.
- Research and Development: The distinction between pemphigoid and pemphigus is crucial to conducting studies and clinical trials relating to these diseases. Research efforts focusing on studying the unique pathophysiology, immunology, as well as treatments for each condition could result in advancements in medical science as well as better outcomes for those suffering from it.
- patient education: Effectively educating patients about their medical condition and the best way to manage it is essential for adhering to treatment plans and self-care. Communication and understanding are clear. the type of disease allows patients to take an active role in the healthcare decisions they make.
The significance of distinguishing between pemphigoid as well as pemphigus is to tailor treatment by predicting prognosis and treatment, avoiding complications, minimizing the effects of side consequences, and ultimately improving the overall health and overall quality of life for patients affected by this auto-immune disease that blisters.
Explanation of autoimmune blistering diseases
Autoimmune blistering conditions (AIBDs) can be described as a class of rare, often fatal medical conditions that manifest as the development of blisters and fluid-filled lesions that appear on the mucous membranes or skin.
These conditions are caused by an abnormal immune response in the body’s immune system. It misguidedly targets and attacks vital proteins that play a vital part in preserving the health of the mucous membranes.
Here’s a more in-depth explanation of the autoimmune diseases that cause blisters:
- The Immune System is Dysfunction: In autoimmune blistering conditions the immune system, which is meant to defend our body from invaders, such as viruses and bacteria, becomes dysfunctional. It creates antibodies (autoantibodies) that specifically target proteins that are essential to adhesion between the skin and the mucous membrane.
- targeted proteins: The principal AIBDs’ targets are desmogleins, desmoplakins BP180, and BP230. These proteins play a role in the functioning and structure of cell-to-cell adhesion inside the mucous membranes and skin. If these proteins get attacked by antibodies the cell-to-cell adhesion weakens which leads to the formation of blisters.
- Clinical presentation: AIBDs may present with a range of clinical signs, such as skin blisters, ruptures, and ulcerations. The blisters may be large or small and deep or shallow and can rupture easily, creating painful sores. mucous membranes such as those that line the throat, mouth, or genitals, can also be affected.
- Different types of AIBD: The following are many kinds of autoimmune blistering disorders which are each distinguished by specific target proteins as well as specific clinical signs. A few of the most popular types are:
- Pemphigus Vulgaris: Targets desmoglein 1 (Dsg1) and desmoglein 3 (Dsg3) proteins.
- Pemphigus Foliaceus: Targets Dsg1.
- Bullous Pemphigoid: It targets BP180 as well as BP230 proteins.
- Cicatricial Pemphigoid is a condition that affects mucous membranes. It is most prevalent in the mouth and eyes.
- Diagnostics: The identification of AIBDs requires a combination of clinical examination including skin biopsy, as well as the use of immunofluorescence tests. Biopsy samples are analyzed under a microscope to detect specific changes. Immunofluorescence tests aid in determining whether there are autoantibodies.
- Treatment: Treatment of chronic autoimmune blistering disorders typically entails immunosuppressive medicines, including corticosteroids and immunosuppressants, the rituximab drug, or intravenous immunoglobulins (IVIG). The aim of treatment is to suppress the immune system’s abnormal reaction and to reduce the formation of blisters.
- Continuous and Recurrent: AIBDs are typically chronic illnesses that are prone to be recurrent in time. A long-term, effective management strategy and constant surveillance by healthcare professionals are vital to treating the condition and avoiding complications.
Autoimmune diseases that cause blisters are complicated and can have a significant impact on the quality of life of a person. Early diagnosis and appropriate treatment are essential to reduce symptoms, prevent complications, and improve the overall health of those who are affected by these diseases.
Biopsy and histopathological examination
Histopathological and biopsy are vital diagnostic procedures in medicine to assess and analyze samples of tissue that are taken from our bodies. These procedures play a vital function in identifying various ailments, such as autoimmune blistering disorders like pemphigoid and Pemphigus.
This article explains how these procedures function and the significance they play in diagnosing these conditions:
Biopsy:
- Definition: The term “biopsies” refers to a procedure that involves removing a small amount of tissue or cells from a particular region of the body to be examined under a microscope. Biopsies are performed on many tissues, including mucous membranes and skin organs, tumors, and organs.
- The purpose of HTML0 is to treat autoimmune blistering Disorders: In the case of autoimmune disease that causes blisters the procedure of a skin biopsy is typically performed to collect samples of tissue from lesions or blisters. The aim is to look at the affected tissue for particular features and anomalies that can assist in identifying the root cause.
- Method: The biopsy procedure usually includes the steps listed below:
- Anesthesia: An anesthetic local to the area is administered to help numb the biopsy site.
- sample collection: A tiny piece of mucous membrane is removed with care by using a scalpel or a biopsy punch.
- Closure: Based on the size and area of the biopsy the wound can be closed using stitches or allowed to heal itself.
Histopathological Examination:
- Definition: Histopathology refers to the examination of tissues on a microscopic scale to determine their composition, structure, and any alterations. Histopathological analysis involves the thorough analysis of sections of tissue to detect any changes or characteristics associated with the disease.
- The purpose of HTML0 is to treat autoimmune blistering Conditions: When there is an autoimmune condition that causes blisters conditions, the tissue sample taken via biopsy is sent to a pathology lab to undergo histopathological analysis. This exam lets pathologists evaluate the structure and cellular changes, particularly seeking out signs of inflammation, blister formation, and the presence of immune-related deposits.
- Process: The steps that are that are involved in histopathological examinations comprise:
- Tissue Processing: The biopsy specimen is processed, fixed, and then embedded in wax to form thin sections that can be examined microscopically.
- Staining: Staining with special stains like hematoxylin and eosin (H&E) as well as immunofluorescence staining, can be used to draw attention to particular structures or features.
- Microscopic Examining: A pathologist inspects the stained tissue sections with microscopes to look for the typical changes and signs of abnormalities.
Significance:
- Histopathological and biopsy examinations are vital in confirming autoimmune diseases by identifying the specific characteristics that are associated with these diseases.
- They aid in identifying various types of autoimmune blistering disorders (e.g. pemphigoid, pemphigoid, and pemphigus) by determining the site of formation of blisters as well as the appearance of specific immune deposits.
- Histopathological studies can aid in the decision-making process for treatment and provide information regarding the severity and progress.
- These processes play an essential function in assessing the activity of disease and the response to treatment over the course of time.
In the end, in summary, histopathological and biopsy examinations are vital tools for the treatment and diagnosis of autoimmune diseases that cause blisters. They help healthcare professionals quickly identify the cause tailor treatment strategies and offer patients the best possible care.
Similarities Between Pemphigoid and Pemphigus
Pemphigoid, as well as pemphigus, are both autoimmune conditions that cause skin irritation as well as mucous membranes. Although they differ in many ways, however, they share some similarities:
- autoimmune Nature: Pemphigoid and pemphigus can be described as autoimmune diseases which means they are the result of an ineffective immune system. In both instances, the immune system creates autoantibodies which attack certain proteins within the body.
- Blister Form: In both conditions, the primary manifestation is the formation of blisters. The blisters may form on the mucous membranes. They can lead to painful ulcers and erosions.
- mucosal involvement: Both pemphigoid and pemphigus are a problem for mucous membranes, such as the ones in the throat, mouth eye, and genital regions. The mucosal involvement could cause discomfort and difficulty talking, eating, or swallowing.
- Diagnose Methods: The approach to diagnosis for both conditions is based on an evaluation of the skin, a biopsy, and immunofluorescence tests. These tests help to identify that there are autoantibodies and determine the specific proteins targeted by the immune system.
- chronic conditions: Pemphigus and pemphigoid are generally chronic diseases and can last over an extended period of time. The treatment for these conditions typically requires regular medical attention and treatment.
- Treatment Method: The specific treatments might be different, the two conditions can be controlled by immunosuppressive medication. Corticosteroids, immunosuppressants, and other medications can be utilized to reduce the autoimmune response and prevent blister formation.
- impact on Quality of Life: Both pemphigoid and pemphigus have the potential to significantly affect a patient’s health and quality of life because of the discomfort, potential for complications, and the long-term nature of these illnesses.
- Possibility of Recurrence: The two diseases may be prone to relapses and recovery, when symptoms get better and then become worse over time. Patients suffering from these conditions could require ongoing monitoring to prevent flare-ups efficiently.
- secondary infections: The skin’s barrier to protect itself is weakening because of erosion and blisters Both conditions increase the chance of secondary infection with a bacterium. The proper care of wounds and prevention of infections is crucial for reducing the risk of these infections.
Although pemphigus and pemphigoid share the same characteristics it is crucial to be aware of their distinct differences in terms of the target proteins and the age of the onset of symptoms since these variables influence the diagnosis, treatment, and prognosis of each.
A precise diagnosis by an expert in healthcare is essential in providing the most effective treatment for patients suffering from these autoimmune conditions that cause blisters.
Reference Books
Certainly! Here are some reference books that cover the topics of autoimmune blistering diseases, including pemphigoid and pemphigus, along with related dermatological and immunological conditions.
These books can be valuable resources for healthcare professionals, researchers, and individuals seeking in-depth information:
- “Autoimmune Bullous Diseases: Approach and Management” by Dedee F. Murrell
- This comprehensive book provides insights into the clinical aspects, diagnosis, and management of autoimmune blistering diseases, including pemphigoid and pemphigus. It covers treatment strategies, immunopathology, and patient care.
- “Blistering Diseases: Clinical Features, Pathogenesis, Treatment” by John T. Seykora, M. Peter Marinkovich, and Wei-Li Di
- This book offers a thorough examination of blistering diseases, including both autoimmune and non-autoimmune conditions. It covers clinical features, immunopathology, and various treatment options.
- “Pemphigus: Basic and Clinical Advances” by Sergei A. Grando
- Focused specifically on pemphigus, this book delves into the pathogenesis, immunology, and clinical aspects of the disease. It also discusses current treatment approaches and emerging research.
- “Autoimmune Blistering Diseases: Part II, An Issue of Dermatologic Clinics” by Dedee F. Murrell and Philip R. Cohen
- Part of the Dermatologic Clinics series, this book focuses on autoimmune blistering diseases, their diagnosis, and management. It includes contributions from experts in the field and offers a clinical perspective.
- “Immunodermatology” by Leslie B. Baumann and Sergey Rezvani
- While not exclusively about blistering diseases, this book provides a broader overview of immunodermatology, including autoimmune conditions affecting the skin. It covers the underlying immunology and practical aspects of diagnosis and treatment.
Conclusion
Pemphigoid and Pemphigus are conditions that cause autoimmune blisters and have some commonalities but have distinct differences in regard to the target antigens, clinical characteristics, and treatment methods.
The distinction between these two conditions is essential to ensure a proper diagnosis and efficient treatment. A timely diagnosis and proper treatment can greatly enhance the quality of life of those affected by these difficult skin conditions. Research and development in medicine continue to help us better understand and treatment for autoimmune blistering disorders.