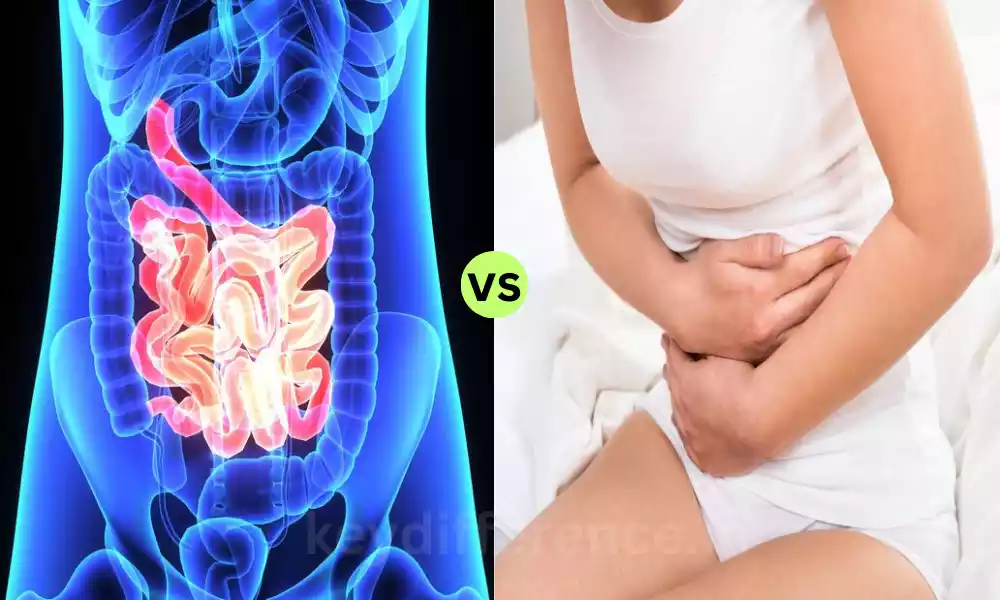
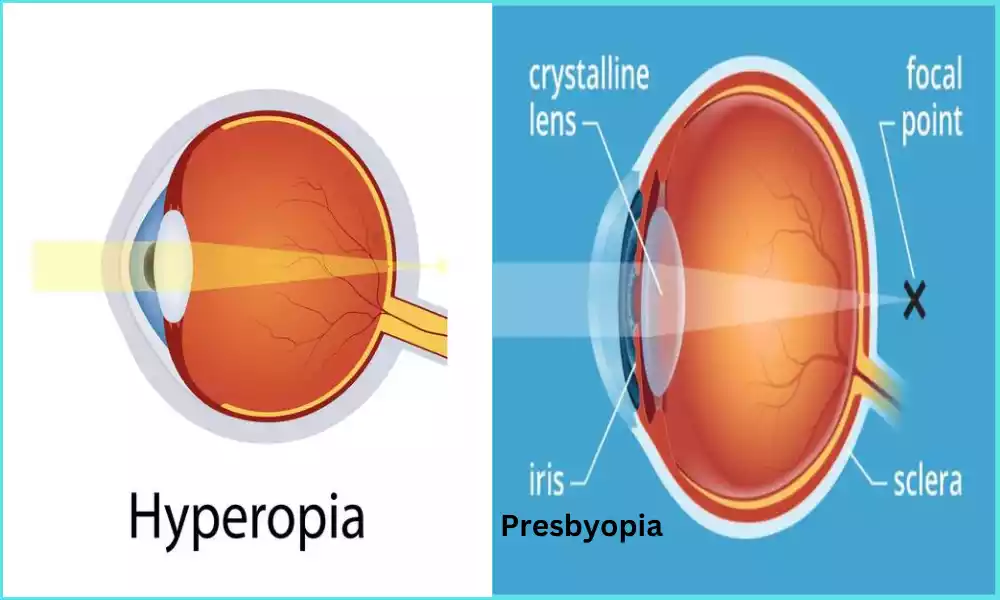
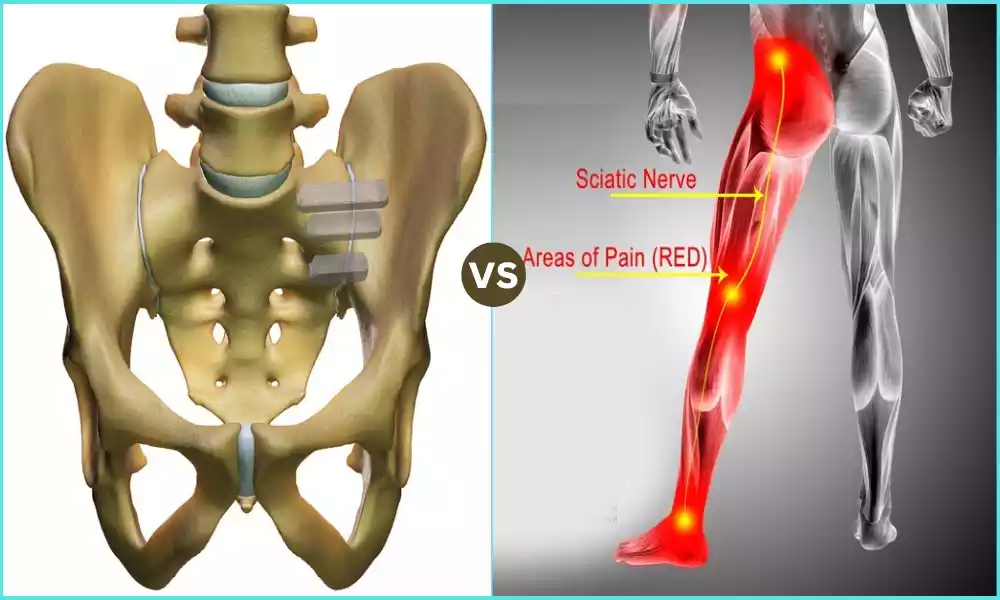
The digestive system of the human body plays an important role in breaking down food items and absorption of important nutrients. But, if the digestive system doesn’t work properly, it could cause conditions such as maldigestion and malabsorption.
While the Malabsorption and Maldigestion terms sound alike they refer to different processes and problems in digestion. Malabsorption is the term used to describe the inability of the intestines to absorb nutrients that have already been digested food. Maldigestion refers to the body’s inability to break down food properly before it gets to the digestive tract. Understanding the difference between these two conditions is essential to identify the cause and a suitable treatment.
What is Malabsorption?
Malabsorption is the inability or impairment in the digestion system, in particular the intestines that absorb some or all of the vital nutrients from food items we eat. This could be caused by various causes, ranging from problems with the inner lining of the intestines to issues with the processes that break down and move substances into the bloodstream.
People who suffer from malabsorption might not receive the maximum benefit from the nutrients they get from their diet and may suffer from deficiency and health issues.

What is Maldigestion?
Maldigestion refers to the body’s inability to properly digest or break down certain nutrients and foods in the digestive tract because of an absence of the necessary digestive enzymes, or other causes.
This means that, even before nutrients make it to the intestines to absorb them they’re not properly digested which could result in foods that aren’t digested in the digestive system, and later problems such as gas, bloating, or nutritional deficiencies.
Importance of proper nutrient absorption and digestion for overall health
Importance of Proper Nutrient Absorption and Digestion for Overall Health:
- Energy Production: Digestion is the process of breaking down carbohydrates, fats, and proteins into more simple molecules such as fatty acids, glucose as well and amino acids. These are the main sources of energy for tissues, cells, and organs.
- Regeneration and Cell Growth: A proper absorption process ensures that vital nutrients are absorbed into cells. These nutrients help in the growth of cells, repair damaged tissues, and aid in the overall function of cells.
- Hormone and enzyme production: Certain nutrients function as precursors for the creation of enzymes and hormones that are vital. For instance, cholesterol is necessary to synthesize the hormone steroid, while zinc plays an important part in the function of enzymes.
- Bone Health: Minerals such as calcium and phosphorus that are absorbed by the intestines, are essential to maintain the density of bones and the health of the skeletal system.
- Cognitive function: Nutrients such as omega-3 fats, antioxidants, as well as specific Vitamins (like B vitamins), are essential to the health of your brain, memory, and cognitive functioning.
- The Immune System’s: proper digestion and absorption of nutrition such as vitamins C, D, and E, zinc, and selenium are crucial for an effective immune response and protection against pathogens.
- Prevention of deficiencies in nutrient intake: Absorption or digestion may cause deficiency, leading to conditions such as anemia (from iron or vitamin B12 deficiency) or Scurvy (from Vitamin C deficiency) as well as Rickets (from the deficiency of vitamin D).
- Maintaining Gut Health: Proper digestion helps maintain a balanced gut microbiome. However, maldigestion could cause imbalances, which can lead to the proliferation of harmful bacteria which may cause conditions such as irritable bowel syndrome and infections.
- Detoxification: The nutrients that are absorbed by our bodies help in the detoxification process of the kidneys and liver aiding in the elimination of waste and toxic substances.
- Preventing Chronic Health Conditions: A proper absorption of nutrients decreases the risk of a range of chronic illnesses. For example, sufficient consumption and absorption of antioxidants may aid in reducing inflammation caused by oxidative stress, which can reduce the chance of certain cancers as well as degenerative diseases.
- Emotional and mental Health: It is clear that there is an immediate link between the absorption of nutrients as well as gut health and the regulation of mood. For instance, the gut is responsible for an important portion of serotonin in the body which is a neurotransmitter that affects mood.
Digestion and the subsequent absorption of nutrients are essential to overall health and well-being. Any disruption in these processes could result in consequences that affect multiple body systems, which highlights the importance of keeping a healthy gut.
Comparison Table of Malabsorption and Maldigestion
Comparison Table: Malabsorption vs. Maldigestion
| Aspect | Malabsorption | Maldigestion |
|---|---|---|
| Definition | The inability of the intestines to absorb nutrients from digested food. | The inability of the body to properly break down food before it reaches the intestines. |
| Stage in Digestion | Occurs after the food is digested, during the absorption phase in the intestines. | Occurs before the absorption phase, during the breakdown of food in the stomach and small intestine. |
| Primary Issue | Absorption of nutrients. | Digestion/breakdown of food. |
| Causes | Inflammatory bowel diseases – Celiac disease – Bacterial overgrowth – Pancreatic insufficiency – Surgical interventions | Insufficient digestive enzymes- Impaired bile release – Certain medications |
| Common Symptoms | Chronic diarrhea – Weight loss – Fatty, foul-smelling stools – Nutrient deficiencies | Abdominal pain – Gas and bloating – Indigestion – Undigested food in stools |
| Diagnosis & Tests | Blood tests – Stool tests – Hydrogen breath test – Endoscopy or biopsy | Blood tests for enzyme levels – Imaging studies – Breath tests |
| Treatment Approaches | Dietary changes – Treat underlying intestinal condition – Vitamin and mineral supplements | Enzyme replacement – Address underlying cause (e.g., gallstone removal) |
This table provides a concise overview of the differences between malabsorption and maldigestion, two conditions that affect the digestive system.
The inability of the intestines to absorb nutrients from digested food
If the intestines are unable to absorb the nutrients that are absorbed from food digested this causes the condition known as malabsorption. Malabsorption can trigger many problems and symptoms, mostly due to the body not receiving the necessary nutrients it requires for proper functioning.
Here’s a deeper look:
Causes of Malabsorption:
- Disorders in the Intestinal Lining: conditions like celiac disease, in which the immune system attacks the lining of the small intestine, in response to gluten intake, may damage the villi (tiny finger-like projections inside the intestines that are responsible for absorption of nutrients).
- Inflammatory Bowel Disorders (IBD): Conditions such as Crohn’s Disease and ulcerative colitis may cause intestinal inflammation, hindering their ability to absorb nutrients.
- Short Bowel Syndrome: The condition is caused by the removal surgically of a substantial part of the small intestinal tract, or due to congenital problems that reduce the surface of absorption.
- The Infections, Bacterial Growth, and Overgrowth: Infections can cause damage to the intestinal lining and bacterial overgrowth may disrupt the normal absorption process.
- Pancreatic disorders: Chronic pancreatitis may result in a decrease in the production of enzymes that are essential to breaking down food, which can lead to malabsorption.
- Bile salt deficiency: Bile salts made through the liver before being stored within the gallbladder, assist in the digestion of fats. Deficiency in them can cause malabsorption of fats.
Symptoms of Malabsorption:
- Chronic diarrhea, usually with a bad smell and a greasy appearance.
- Weight loss even when your diet is healthy or higher.
- Insomnia and fatigue.
- Gas and gas bloating.
- Abdominal discomfort.
- Appetite changes.
- Mineral and vitamin deficiencies can lead to osteoporosis and anemia as well as skin diseases.
- Swelling (edema) because of the malabsorption of proteins.
Diagnostics: Healthcare providers may use a variety of tests to detect malabsorption, for example:
- Tests on the stool to find fat content.
- The tests of blood can reveal nutritional deficiencies.
- Breath tests are used to determine issues like lactose intolerance or the presence of bacterial growth.
- Imaging tests, such as X-rays and CT scans.
- Endoscopy, with biopsy, to check the intestinal liner.
Treatment:
- Finding the root cause of the issue is essential. For instance, with celiac disease adherence to a gluten-free diet is required.
- Adjustments to your diet, like cutting down on fat consumption or adhering to the lactose-free diet.
- Supplements to replace minerals and vitamins.
- If needed, replace enzymes with a replacement.
It’s crucial to detect and treat malabsorption as early as possible since chronic deficiencies in nutrients can have long-term detrimental consequences for overall health.
Insufficient production of digestive enzymes
If the body is producing a low quantity of digestion enzymes it could lead to the condition known in the form of “enzymatic insufficiency” or “pancreatic enzyme insufficiency.” These enzymes are crucial to break down food ingredients such as proteins, fats, and carbohydrates within the digestive tract, and ensuring their form that is able to be taken up through the intestinal tract.
Causes of Insufficient Production of Digestive Enzymes:
- Chronic Pancreatitis: The inflammation of the pancreas for a prolonged time can cause damage to its cells, resulting in a lower production of digestive enzymes.
- Cystic Fibrosis: is a genetic condition that affects a variety of body systems including the pancreas, which causes mucus accumulation that may block the pancreatic enzymes’ release.
- Pancreatic Cancer: The tumors may interfere with the pancreas’s normal functions.
- Shwachman Diamond Syndrome: The condition is a rare genetic disorder that affects the pancreas, as well as bone marrow.
- Aging: The natural decrease in the production of digestive enzymes may occur as we age.
- Post-pancreatectomy: removal or surgical modification of the pancreas may decrease its enzyme-producing capacity.
- Certain medicines: Certain medications may influence the production of enzymes or secretion.
Symptoms of Insufficient Production of Digestive Enzymes:
- A feeling of fullness following eating
- Bloating and gas
- Pain or discomfort in the abdomen
- The stools are floaty, fat stool, or sour-smelling (steatorrhea)
- Unintentional weight loss
- Malabsorption of nutrients that leads to deficiencies
- Diarrhea or frequent, loose stool
Diagnosis:
- Fecal Elastase Testing: The test measures what amount of elastase an enzyme for digestion present in stool.
- The Fecal Fat Test: Tests the content of fats in stool to determine if there is malabsorption is taking place.
- Testing for Blood: to determine nutritional deficiencies.
- Imaging Studies: Similar to CT scans and MRIs to examine the pancreas.
Treatment:
- Pancreatic Enzyme Replacement Therapy (PERT): Supplements that provide the essential digestive enzymes. They are usually taken along in conjunction with meals to help digestion.
- Food Adjustments: Consuming easy-to-digestible food items or smaller, less frequent meals.
- Vitamins And Mineral Supplements: To treat any deficiencies that result from malabsorption.
- The Treatment of the Cause: This may involve controlling chronic pancreatitis adjusting the medications that cause the problem or addressing other conditions that are primary.
Making sure that food items are correctly broken down is vital for the absorption of nutrients and overall health. If enzyme production is affected this can cause numerous health problems and discomforts, which is why it’s essential to tackle the issue quickly.
Similarities Between Malabsorption and Maldigestion
While maldigestion and malabsorption are distinct digestive conditions They do have certain similarities, especially in relation to their effects on the overall health of your digestive system.
Here are some similarities between maldigestion and malabsorption:
- Digestive System Involvement:
- Maldigestion and malabsorption are both digestive conditions that impact how nutrients are absorbed by the body.
- Both can cause various digestive issues, and they could be overlapping.
- Gastrointestinal Symptoms:
- Both of them can trigger stomach-related symptoms, such as abdominal discomfort, bloating, and changes in bowel habits and bowel movements, such as diarrhea.
- Nutritional Deficiencies:
- Maldigestion and malabsorption can result in nutritional deficiencies as they affect the body’s ability to absorb essential nutrients.
- Common problems in both conditions can comprise vitamins (e.g. B vitamins,) as well as minerals (e.g. iron, calcium).
- Impact on Weight:
- Maldigestion and malabsorption can result in weight loss that is not intended because of decreased absorption of nutrients and a decrease in the utilization of calories.
- Secondary Health Complications:
- Both conditions could result in secondary health consequences in the event of untreated conditions or the root causes of the problem aren’t treated.
- For instance, osteoporosis or anemia is common in those who suffer from maldigestion or malabsorption due to nutritional deficiency.
- Diagnosis:
- Maldigestion and malabsorption both need similar tests for diagnosis such as stool tests, blood exams, imaging research, and occasionally biopsies to determine the root causes and extent of the problem.
- Treatment Approaches:
- Certain aspects of the treatments for malabsorption as well as maldigestion could overlap. Both conditions can require dietary adjustments and nutritional supplements.
- In some instances, both conditions could be helped by medication or enzyme replacement therapy to treat certain symptoms.
It is important to remember that, despite some similarities, the major difference between maldigestion and malabsorption is in their root reasons and the place where the digestive malfunction is observed. Malabsorption is primarily a problem with the absorption of nutrients in the small intestine.
On the other hand, maldigestion is a result of difficulties breaking down food within the stomach or in the small intestine. So, the appropriate treatments and strategies for managing the condition will differ based on the root cause of the disease.
Ultrasound or MRI for gallbladder evaluation
Both ultrasound as well as MRI (Magnetic Resonance Imaging) are a method to evaluate gallbladders, however, the decision between them is contingent on a variety of aspects, such as the particular medical situation, availability, and considerations for the patient.
Here’s an overview with ultrasound and MRI for gallbladder examination:
- Ultrasound for Gallbladder Evaluation:
- Speed: Ultrasound is a speedier and easier-to-access imaging method. It is able to be used in bedside settings and in an outpatient environment, making it a great option for initial assessments.
- Price: Ultrasound is generally less costly than MRI and could play a role in the healthcare decision-making process.
- Effectivity: Ultrasound is highly effective in assessing gallstones that are common that affect the gallbladder. It also helps to determine the dimensions as well as the shape and size of the gallbladder.
- The procedure is non-invasive: Ultrasound can be described as a non-invasive procedure that doesn’t make use of ionizing radiation. This makes it safe for the majority of patients even pregnant women.
- MRI for Gallbladder Evaluation:
- Advanced imaging: MRI provides more precise photographs of the gallbladder as well as the surrounding structures. It may provide better images of soft tissues. This makes it a useful tool for detecting any problems that are not related to gallstones like tumors, inflammation, or functional problems.
- Contrast Enhancement: Contrast agents may be utilized together with MRI to increase the clarity of specific gallbladder problems.
- Patients Considerations: An MRI procedure is a good option when the results of ultrasound aren’t conclusive, or patients are unable to be able to undergo ultrasound (e.g. due to obesity, or excessive stomach gas).
- Functional Assessment: Techniques for functional MRI are able to evaluate gallbladder motion as well as function. This is vital in cases of biliary dyskinesia, for example.
The decision between ultrasound and MRI for gallbladder examinations is contingent on the context of the patient and the particular information required. Ultrasound is typically the first-line imaging option because of its accessibility as well as its cost-effectiveness and capability to identify gallstones.
MRI is generally reserved for instances where more details or more information is required, or if the results of ultrasound are not conclusive. The decision must be taken by the medical professional according to the patient’s requirements and the probable or established condition of gallbladder.
Conclusion
Both ultrasound as well as MRI are excellent imaging instruments for gallbladder examination. Ultrasound is efficient, economical, and effective in detecting gallstones.
MRI is, on the contrary, more detailed imaging and can be useful in assessing the gallbladder’s function. The decision between these two is based on the specific clinical scenario and the information that is required to make a correct diagnosis and treatment plan.