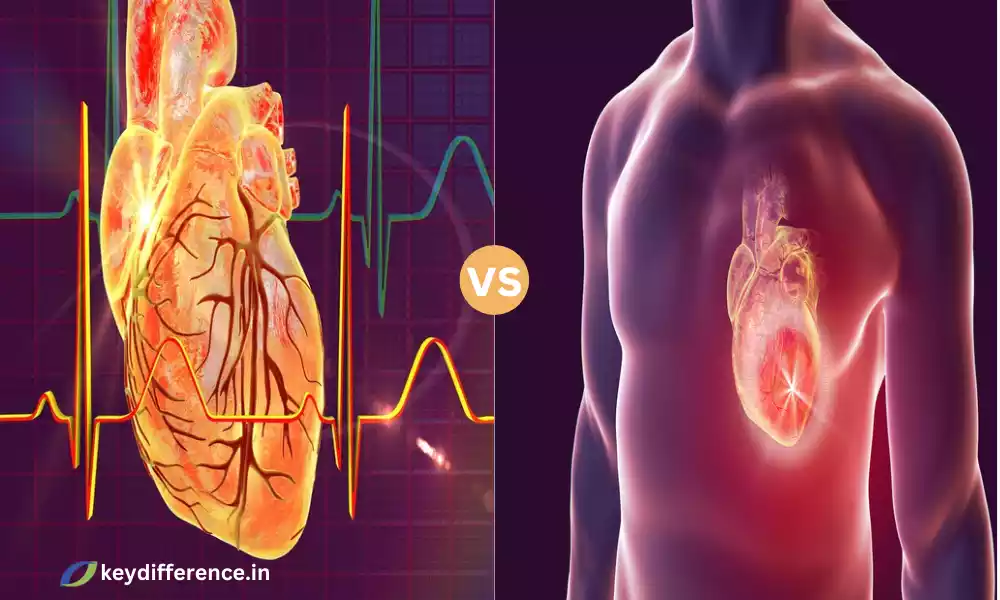
Left Ventricular Hypertrophy and Hypertrophic Cardiomyopathy are two heart conditions that are characterized by an increase in the thickness of heart muscles. Although they have some commonalities they differ in origin, presentation in the clinic, and treatment.
These distinctions aid health professionals and patients in discerning the difference between LVH and HCM to make a precise diagnosis and proper treatment.
Explanation of Left Ventricular Hypertrophy
LVH is a term used to describe the condition of left ventricle hypertrophy (LVH) is an illness in which the muscular wall of the left ventricle, which is the primary chamber that pumps the heart, is abnormally in size or thickened.
The thickening of the wall is usually caused by increased demands on the heart. This is usually because of conditions such as hypertension (hypertension) and aortic valve disorder or other cardiac conditions.
LVH could be a compensatory mechanism that helps take on the additional demands of the heart however it can also cause diminished heart function if left untreated. It is usually diagnosed with ultrasound imaging and is a significant clinical sign that needs further investigation and treatment.

Explanation of Hypertrophic Cardiomyopathy
Hypertrophic Cardiomyopathy (HCM) is a heart disease that is genetically caused by an abnormal growth (hypertrophy) in the muscle of your heart, especially the left ventricle. It is not accompanied by an obvious cause, like the presence of high blood pressure, or valve diseases.
In HCM the heart muscle is larger than normal. This could disrupt normal heart functioning, hinder the flow of blood out of the heart, and lead to a myriad of complications and symptoms.
HCM is predominantly an inheritable condition that is caused by mutations in genes that alter the structure of the cardiac muscle proteins. It is the leading cause of sudden cardiac death among athletes and young people so early detection and proper treatment are essential for those suffering from HCM and their families.
Comparison Table of Left Ventricular Hypertrophy and Hypertrophic Cardiomyopathy
Here’s a comparison table highlighting the key differences between Left Ventricular Hypertrophy (LVH) and Hypertrophic Cardiomyopathy (HCM):
| Aspect | Left Ventricular Hypertrophy (LVH) | Hypertrophic Cardiomyopathy (HCM) |
|---|---|---|
| Definition | Thickening of the left ventricle wall due to increased workload or other cardiac conditions | A genetic condition characterized by abnormal thickening of the heart muscle without an apparent cause |
| Etiology | Often secondary to conditions like hypertension, aortic stenosis, or other cardiac disorders | Primarily caused by genetic mutations affecting cardiac muscle proteins |
| Genetic Component | Typically not genetic in origin | Inherited as an autosomal dominant trait, with a familial occurrence |
| Clinical Presentation | Often asymptomatic or presents with symptoms related to underlying conditions (e.g., hypertension) | Variable symptoms, including chest pain, dyspnea, syncope, or sudden cardiac death |
| Diagnosis | ECG changes, echocardiography, and imaging may reveal LVH | ECG abnormalities (e.g., Left ventricular hypertrophy), echocardiography, and genetic testing |
| Complications and Prognosis | Associated with underlying cardiac conditions and can lead to heart failure | Risk of arrhythmias, sudden cardiac death, and heart failure may develop |
| Treatment | Management focuses on treating the underlying cause (e.g., hypertension) and symptom relief | Medications (beta-blockers, calcium channel blockers), implantable devices, and surgical interventions |
| Lifestyle Modifications | Blood pressure management, diet, and exercise control | Avoidance of strenuous exercise; genetic counseling for family members |
| Common Population Affected | Prevalent in individuals with hypertension or other cardiac conditions | Genetic conditions affecting a broader population, including athletes |
| Age of Onset | Typically seen in older adults with underlying cardiac issues | Can present at any age, including in young individuals |
| Risk of Sudden Cardiac Death | Generally lower risk compared to HCM | Higher risk, particularly in young individuals and athletes |
This table summarizes some of the key differences between LVH and HCM, including their causes, clinical features, diagnostic methods, and management approaches.
It’s important to note that both conditions involve thickening of the heart muscle but have distinct underlying causes and clinical implications.
Importance of understanding the differences between LVH and HCM
Understanding the difference between Left Ventricular Hypertrophy (LVH) and Hypertrophic Cardiomyopathy (HCM) is of vital importance for a variety of reasons:
- Accurate diagnosis and treatment: Distinguishing between LVH and HCM is essential in order for healthcare professionals to give an appropriate and efficient treatment. LVH could be a result of underlying causes like hypertension which require a different approach to management in comparison to the genetic causes of HCM. Incorrect diagnosis can result in inappropriate treatment, and possibly damage.
- Risk assessment: Understanding the risk profile differences of LVH as well as HCM is crucial. HCM for instance, has a higher risk of sudden cardiac death, particularly in athletes and young people. Recognizing HCM in these populations could be a trigger for specific surveillance and preventive actions.
- Genetic Counseling: It is an inherited disorder that has a familial inheritance pattern. An accurate diagnosis aids in identifying affected relatives who could receive genetic counseling and tests. This allows for early detection and treatment.
- Lifestyle Recommendations: Exercise and lifestyle modification recommendations differ considerably in LVH as well as HCM. Being aware of these distinctions will help prevent any potential problems, particularly when it comes to HCM which is a condition where intense exercise is dangerous.
- The Prognosis, as well as the Long-Term Plan: Understanding the natural course of each illness and the prognoses for each is vital in long-term planning as well as patient education. Patients suffering from LVH might be on a different trajectory and outlook than those who suffer from HCM.
- Studies as well as Advancements: Accurate differentiation between these disorders aids clinical research as well as developing targeted treatments. Researchers can concentrate their efforts on understanding the particular aspects and genetic causes of HCM which could lead to better treatments and treatments.
- Public Health: Public awareness campaigns can assist people in understanding the importance of maintaining a healthy heart and the distinctions between different cardiac conditions. This awareness could result in earlier detection and improved results.
- Preventive measures: Understanding the differences could result in preventive measures. For instance, knowing the genetic cause of HCM could motivate relatives to have genetic tests and then take steps to control their heart health more effectively.
knowing the differences in LVH as well as HCM is crucial to ensure a precise diagnosis, the right treatment as well as the assessment of risk, counseling genetic lifestyle advice, and future planning for the long term, study, and the public’s awareness.
This ultimately leads to better outcomes for patients and better overall care for patients with heart disease.
Physiological response to increased cardiac workload
This physiological response to an increased heart workload, for example during exercise or as a response to certain medical conditions includes a variety of intricate mechanisms aimed to ensure that the heart is able to meet the body’s growing demands for nutrients and oxygen.
This is controlled via the system for autonomic nerves, as well as hormonal signals.
Here’s a brief overview of major physiological reactions:
- An Increased heart rate (Heart Rate Increase): One of the first reactions to increased heart workload is an increase in the heart rate. It is because the sinoatrial (SA) node inside the heart creates electric signals that are generated at a greater rate, resulting in a greater frequency of contractions. This lets the heart pump more blood every minute.
- Increased Stroke Volume: Stroke volume is the quantity of blood released from the left ventricle in every heartbeat. In times of increased workload, the heart pumps more vigorously, thereby increasing the volume of stroke. This is achieved by greater heart rate and contraction of the ventricular muscles, as well as the release of blood.
- Advanced Cardiac Output: Output from the heart is the result of the heart’s rate as well as stroke volume. It is the volume of blood that the heart pumps out per minute. When both the stroke volume and heart rate rise the cardiac output increases to meet the increasing need for nutrients and oxygen from organs and tissues of the body.
- Vasodilation: The blood vessels in the body, especially the arterioles, expand due to an increase in workload. Vasodilation lowers peripheral vascular resistance, which makes it simpler for heart muscle to pump blood into the circulation system. This allows for the flow of blood to all tissues in the body.
- Increased Contractility: The myocardium (heart muscle) is more flexible when working at a higher intensity. This is because of the sympathetic nervous system’s release of norepinephrine which increases the force in myocardial muscle contractions. In turn, the heart pumps faster.
- Redistribution of Blood Flow: The flow of blood is distributed to focus on the needs of various organs and muscles when there is greater work. For instance, more blood flow is directed to the muscles of the skeletal system and away from the digestive system when exercising.
- Increased Oxygen Extraction: Muscles and tissues extract oxygen from the blood more effectively when they are in high activity. This is achieved by increasing the speed of oxygen transport through the bloodstream into cells.
- The release of hormones that cause stress: Your adrenal glands produce stress hormones, such as epinephrine (adrenaline) in times of greater cardiac workload. These hormones can also boost the heart rate, contractility, and overall performance of the heart.
- Respiratory Rate Rises: In response to an increase in cardiac workload the rate of breathing rises. This ensures that the body is getting enough oxygen to meet the increasing metabolic demands.
- Regulating the blood Pressure: The body closely regulates blood pressure in an increase in cardiac workload, to avoid excessive rises. Baroreceptors, along with other mechanisms, help keep the blood pressure at a safe level.
These physiological reactions collectively allow the heart to adjust to higher demands, for instance, when stressed or exercising as well as ensure the body is receiving enough oxygen and nutrients in order to meet the needs of metabolism.
Genetic mutations affecting myocardium
Genetic mutations that affect the myocardium (the muscle part of the heart’s wall) can cause a variety of heart conditions and disorders. These changes typically result in changes in the genes that are responsible for the cardiac muscle’s structure and function.
Here are a few examples of genetic changes that may affect the myocardium:
- Hypertrophic Cardiomyopathy (HCM): HCM is primarily caused by mutations in genes that encode sarcomere proteins that are crucial for the contraction of cardiac muscle. Genes with mutations such as MYH7 (beta-myosin heavy chain) and MYBPC3 (myosin-binding protein C) can cause abnormal thickening of the myocardium that is seen in HCM.
- Dilated Cardiomyopathy (DCM): DCM can also be genetically based. Genetic mutations in genes like TTN (titin), LMNA (lamin A/C), and Desmin (desmin) could weaken the myocardium, resulting in an increase in the size of heart chambers as well as diminished contractile function.
- Arrhythmogenic Right Ventricular Heart Disease (ARVC): ARVC is a condition in which the myocardium in the right ventricular region is replaced with fibrous and fat-filled tissue. Genes with mutations like PKP2 (plakophilin-2) or DSG2 (desmoglein-2) can be connected with ARVC and can disrupt normal cardiac cell junctions.
- Familial Dilated Cardiomyopathy (FDC): Some forms of DCM have a significant genetic component that can be found within families. Gene mutations like TNNT2 (troponin T) and ACTC1 (cardiac alpha-actin) have been associated with FDC.
- Restrictive Cardiomyopathy (RCM): RCM may result from genetic mutations that affect the proteins that are involved in myocardial compliance. Genes that are affected by mutations like TNNI3 (troponin I) and MYL2 (myosin light chain 2) can cause an abnormal stiffness of the myocardium.
- Left Ventricular Compaction Cardiac Myopathy (LVNC): LVNC is distinguished by the spongy appearance of the myocardium. Genetic mutations, most often in the myocardial complication genes in the course of the development (e.g. MYH7 and the ACTC1 gene) may cause LVNC.
- Arrhythmias: Genetic mutations can cause a variety of arrhythmias that occur in the cardiac system. For instance, Long QT Syndrome (LQTS), Brugada Syndrome, and Catecholaminergic Polymorphic Ventricular Tachycardia (CPVT) are caused by mutations in the genes that code for Ion channels or channel-related proteins within the myocardium.
- Channelopathies: A few genetic diseases like Hypertrophic Cardiomyopathy (CMH1) are caused by genetic mutations that affect genes that regulate Ion channel function within the myocardium. These mutations could disrupt normal electrical signaling within the heart.
Understanding the genetic mutations that affect myocardium is vital to the diagnosis and treatment of different cardiac ailments. Genetic tests and counseling play a crucial function in identifying those at risk, offering individualized treatment options, as well as providing insights into the screening strategies for families and prevention strategies.
Symptoms may include chest pain, shortness of breath, and fatigue
The signs of chest discomfort, shortness of breath, and fatigue could be a sign of a variety of medical conditions, such as heart and non-cardiac conditions. These symptoms could be indicative of a variety of issues, and it’s crucial to think about the context and any other factors when evaluating the importance.
This is a brief description of how these symptoms may relate to the health of your heart:
- chest pain (Angina): Chest pain, which is often described as a pounding or a squeeze inside the chest could be an indication of decreased oxygen flow in the muscle of your heart, a condition referred to as angina. Angina can be provoked by physical activity or emotional stress, and it is relieved with rest or medication such as Nitroglycerin. It could be a sign of coronary artery disorder (CAD) which is when the coronary arteries are narrowed or blocked.
- Shortness of breath (Dyspnea): Shortness of breath is a typical sign of heart-related problems. It may occur when you are physically active (exertional dyspnea) or even during the time of rest (resting dyspnea). Conditions like heart failure, heart valve diseases, and arrhythmias that are specific to certain conditions can cause dyspnea due to the heart’s inability to pump blood efficiently.
- Fatigue: The term “fatigue,” or extreme tiredness, could be a non-specific symptom relating to various cardiac disorders. In the case of heart failure, a reduced cardiac output can cause fatigue because the body does not get enough nutrients and oxygen. Other cardiac problems like arrhythmias, or coronary artery disease, could be a contributing factor to fatigue.
It’s crucial to understand that these symptoms aren’t solely related to heart issues and may be caused due to other health conditions, too, and include respiratory issues and anxiety as well as muscle-skeletal disorders. Furthermore, some people may suffer from atypical or less frequent symptoms associated with cardiac events, including nausea dizziness, nausea, or radiating into the arm or jaw.
When you, or anyone else you know suffers from chest discomfort, shortness of breath, or fatigue, particularly in the case of persistent, extreme, or accompanied by any other symptoms that are concerning It is crucial to seek medical attention right away.
A prompt evaluation and diagnosis is crucial to identify the root reason and begin the appropriate treatment. Heart-related symptoms shouldn’t be overlooked, since they could be a sign of a life-threatening situation that requires urgent intervention.
Associated with hypertension and other cardiac conditions
The condition known as Left Ventricular Hypertrophy (LVH) is usually related to hypertension (high blood pressure) and various other cardiac issues.
Here’s a more detailed analysis of these relationships:
- Hypertension (High Blood Pressure): LVH frequently is triggered by high blood pressure that is persistently elevated. The left ventricle in the heart performs harder work to pump blood in response to increased resistance within the arterial.As time passes, this increased workload could cause the muscular walls of the left ventricle of the heart to thicken and eventually lead to LVH. The control and management of blood pressure by making lifestyle adjustments and medication is vital to the prevention or treatment of LVH that is associated with hypertension.
- Aortic Stenosis: Aortic stenosis is a heart valve problem that causes the aortic valve to not fully open, thus reducing the supply of blood through the left ventricle to the Aorta. This could lead to increased pressure in the left ventricle. This can cause LVH since the heart muscle gets thicker to get rid of the obstruction.
- Other Heart Diseases of the Valvular Heart: Various valvular heart conditions, like regurgitation or mitral stenosis, may also cause LVH. These conditions alter normal blood flow patterns in the heart, which can result in an increase in pressure or volume in the ventricle left.
- Coronary Artery Disease (CAD): Coronary artery disease, is defined by the narrowing or blocking of coronary arteries. It can decrease blood supply to heart muscles. As a result of this, the left ventricle could be enlarged as it attempts to make up for the decreased nutrition and oxygen supply to the myocardium.
- Cardiomyopathies Some types of cardiomyopathies like hypertensive cardiomyopathy, can result in LVH. These conditions cause functional and structural changes in the muscle of the heart, such as hypertrophy. They are usually connected with chronic hypertension.
- Obstructive Sleep Apnea: People with sleep apnea with obstruction which is a condition that causes sleeping breathing that be interrupted or sleep, can develop LVH due to an increase in blood pressure as well as changes in oxygen levels which strain the heart.
- Obesity The presence of obesity is a danger of hypertension and LVH. Body weight excess could lead to hypertension which in turn causes LVH. Lifestyle changes and weight management are vital to combat this relationship.
It’s important to realize that LVH could have serious consequences on cardiac health since it could lead to arrhythmias, heart failure, or other issues if left untreated.
Thus, people suffering from LVH particularly when it is related to hypertension or other cardiac disorders must receive proper medical treatment, which could include the control of blood pressure, medications, and lifestyle changes to prevent heart-related issues from occurring.
Regularly checking in with a health professional is vital to keep track of conditions and maintain proper cardiovascular health.
Similarities Between Left Ventricular Hypertrophy and Hypertrophic Cardiomyopathy
Left Ventricular Hypertrophy (LVH) and Hypertrophic Cardiomyopathy (HCM) have some commonalities that are primarily due to the growth of myocardium (heart muscle). It is important to remember that although they might share some characteristics, the two conditions also have distinct distinctions.
Here are a few similarities between LVH and HCM:
- Myocardial Thickening: Both LVH and HCM are characterized by the abnormal thickening of the myocardium, especially on the left ventricle within the heart. The thickening is evident through imaging studies, for example, echocardiography.
- Increased Ventricular Mass: In both instances, you will notice an increased volume of the left ventricle. This is due to the thickening of ventricle walls, which can be assessed using imaging methods.
- Cardiac hypertrophy: HCM and LVH are both considered to be forms of cardiac hypertrophy. In each, your heart muscles undergo structural change and become larger and more muscular than it normally is.
- Possibility of symptoms: Both conditions can result in symptoms caused by an impaired function of the heart. These symptoms can include chest discomfort, breath shortness, and fatigue.
- Risk of complications: HCM and LVH may be both associated with a higher risk of cardiac problems. They could be caused by arrhythmias (abnormal heart rhythms) heart failure and, in a few instances, sudden cardiac death.
- Genetic Cause: While LVH is usually a result of conditions such as hypertension, it could be a genetic issue in some instances, particularly when there is a familial background of LVH. HCM however, contrary to what you might think is mostly a genetic disorder that has a significant genetic inheritance pattern that is familial.
- Diagnose Methods: The same diagnostic methods such as electrocardiography (ECG or EKG) and echocardiography are used to determine the function of both LVH and HCM. These tests assist in assessing the heart structure and function.
- Management Strategies: In some cases, the management strategies used to treat LVH and HCM could overlap. Lifestyle modifications, medications, and monitoring are the strategies that are used to treat both conditions, but the particular treatments differ depending on the reason.
It’s crucial to understand these commonalities, however, it is equally crucial to know the distinctions between LVH and HCM due to their distinct causes, genetic components as well as clinical manifestations and prognoses. A precise diagnosis and proper treatment are essential to provide the most effective treatment for those suffering from these diseases.
Reference Books
Certainly! Here are some reference books covering various topics and genres that you might find useful depending on your interests:
Non-Fiction
- Science and Nature:
- “A Short History of Nearly Everything” by Bill Bryson
- “Sapiens: A Brief History of Humankind” by Yuval Noah Harari
- “The Immortal Life of Henrietta Lacks” by Rebecca Skloot
- History:
- “A People’s History of the United States” by Howard Zinn
- “The Guns of August” by Barbara W. Tuchman
- “The Wright Brothers” by David McCullough
- Philosophy:
- “Meditations” by Marcus Aurelius
- “The Republic” by Plato
- “The Genealogy of Morals” by Friedrich Nietzsche
- Biography and Memoir:
- “Steve Jobs” by Walter Isaacson
- “The Diary of a Young Girl” by Anne Frank
- “The Glass Castle” by Jeannette Walls
- Self-Help and Psychology:
- “Thinking, Fast and Slow” by Daniel Kahneman
- “The Power of Habit” by Charles Duhigg
- “Man’s Search for Meaning” by Viktor E. Frankl
Conclusion
An array of reference books that span a variety of categories and topics gives readers the opportunity to discover all the depths of human understanding and creativity.
If you are looking to broaden your knowledge of the world via non-fiction or explore the realm that is fiction-based, the books offer openings to different perspectives, ideas, and concepts.
Reading is a valuable instrument for education, entertainment as well and personal growth which makes these reference books invaluable companions in your journey to knowledge.